Fact Check My Feed: More Kids Can Get COVID-19 Vaccines. Now What?
29:24 minutes
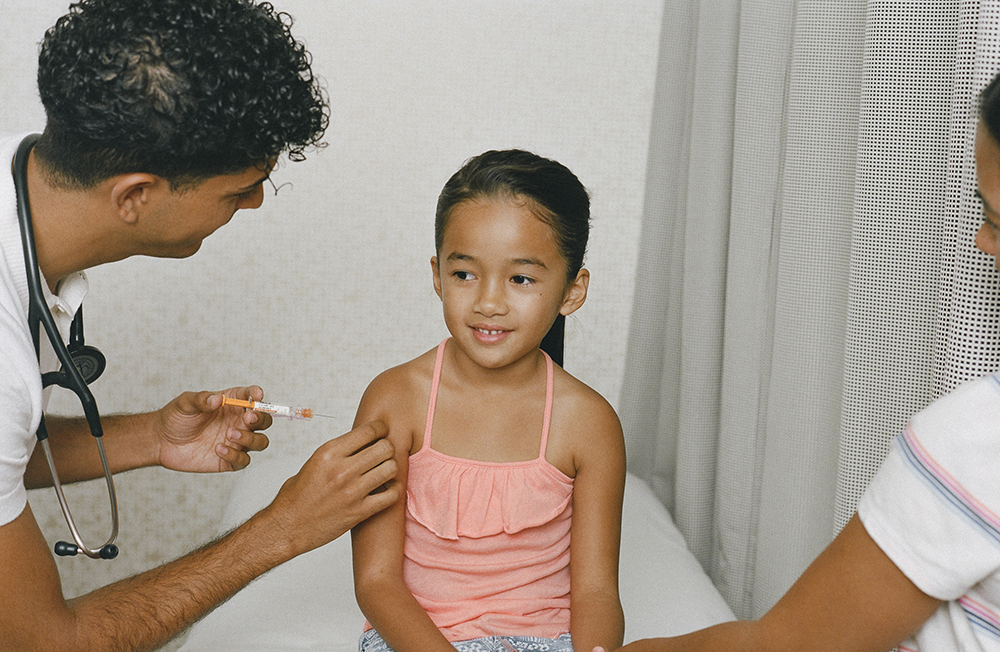
This story is a part of Science Friday’s coverage on the novel coronavirus, the agent of the disease COVID-19. Listen to experts discuss the spread, outbreak response, and treatment.
Many parents around the U.S. breathed a sigh of relief—or an even more intense emotional reaction—at the long-awaited news that the Centers for Disease Control and Prevention (CDC) had signed off on advising the Pfizer-BioNTech COVID-19 vaccine for children aged 5 to 11 this week. The recommendation came after a unanimous vote from the agency’s committee of outside vaccine experts. And last week, the Food and Drug Administration (FDA) authorized the shot after a review of clinical trial data found both low risk and high efficacy in a smaller, kid-calibrated dose of the vaccine.
University of Saskatchewan virologist Angela Rasmussen joins Ira to look at the data behind the FDA’s long-anticipated decision. They also discuss the rationale behind booster shots for high-risk adults, what it means that deer in Iowa have been caught transmitting the virus, COVID-pragmatic holiday planning, and other pandemic news.
This week, Science Friday celebrated 30 years on the air!
We are overwhelmed with gratitude for these 30 incredible years of awe-inspiring and honest conversations with scientists, researchers, writers, policy-makers, educators, and experts. And immensely grateful for you, for 30 years of listener calls and questions that have encouraged our curiosity and driven our programming. Sharing our time with you each Friday has been a gift. Thank you!
But there is more work to do, more stories to be told, and more research to be explored.
Listeners support our work by making donations—big or small. By making a gift, you help us prepare for our future, protect us from uncertainty, and enable us to take risks like launching a new podcast, offering a free event, and providing free educational materials.
The need for fact-based science news is undeniable. Make a donation today, celebrate our 30-year history and be a champion of the next 30 years ahead!
Your support makes a difference.
Thank you,
Ira Flatow and the Staff and Board of Science Friday
Angela Rasmussen is a research scientist at VIDO-InterVac, the University of Saskatchewan’s vaccine research institute in Saskatoon, Saskatchewan.
IRA FLATOW: This is Science Friday. I’m Ira Flatow. A bit later in the hour, we’ll talk about good news for reducing methane emissions from cows. But first, many parents sighed in relief earlier this week when the CDC officially signed off on a recommendation recommending the Pfizer BioNTech vaccine for children aged 5 to 11. The FDA authorized the shot after finding evidence in the– excuse me– in the clinical trial data that the shot was both safe and highly effective in preventing severe diseases.
And again, many parents had been champing at the bit to get their younger children vaccinated. But where does that leave parents who might still have reservations? Are you among them? Here to talk through the safety, the efficacy, and the whys is virologist Angela Rasmussen for another edition of Fact Check My Feed. Let me formally introduce her. Dr. Angela Rasmussen is a research scientist at VIDO-InterVac at the University of Saskatchewan’s Vaccine Research Institute in Saskatoon, Saskatchewan. Welcome back, Angela.
ANGELA RASMUSSEN: Thanks for having me, Ira. It’s great to be here.
IRA FLATOW: And it’s a special day today because we want your COVID-19 suggestions. If you’re listening, yes, you can call us in the studio. 844-724-8255. 844-SCI-TALK. Operators are standing by, as they used to say.
Well, Angela, nice to have you back. Let’s talk– I already mentioned the big news this week is vaccines for younger children. And we want to talk about that. But first before we get to vaccinations, I want to talk about a story that just broke today about a second antiviral pill. Pfizer says it has a pill that is very effective in combating the virus and people who are infected, cutting hospitalizations and deaths by almost 90% in people in high-risk groups. That must be good news, Angela.
ANGELA RASMUSSEN: It’s terrific news. I mean, every time we develop a new countermeasure that we can deploy and have as an option in our back pocket, that’s a real win for everybody’s health and for ending this pandemic. I think what is important to keep in mind is that this isn’t a substitute for vaccination.
But for those people who haven’t been vaccinated, or don’t respond well to vaccines, or get a breakthrough infection in those rare cases where people get severely ill, it’s wonderful to have a treatment like this that also is an oral treatment. So people don’t have to go get infused with it. They can just get a prescription and take it from home. This is a real game-changer in terms of our ability to treat people who have COVID-19.
IRA FLATOW: So even if you get a breakthrough infection, it might be– you just go take a pill?
ANGELA RASMUSSEN: That’s exactly right. And what’s nice about this is we know from all the other antivirals that are out there– Remdesivir, as well as the drug that’s been developed by Merck, Molnupiravir– I still have trouble saying that.
[LAUGHTER]
We know that– and the monoclonal antibodies– we know that early treatment is really, really much more effective. And prior to the drugs from Merck and Pfizer being developed, the only antiviral treatments that were available are treatments that have to be given by intravenous infusion, which means that typically you can’t treat as many people and you can’t treat them as early in the course of their infection, because a lot of times you’re waiting to see who really needs the treatment.
With a pill, that’s a lot easier. People can administer it themselves. There won’t be as many supply issues. So you can give it to everybody essentially who’s diagnosed with SARS-coronavirus-2 infection. They can take it at home and then we don’t have to wait and see who’s actually going to get very sick and need the treatment, because it will keep people from getting very, very sick.
IRA FLATOW: That’s great news. Let’s move on to our main story this hour about vaccinations. I’m sure many folks have questions about the safety of vaccines for younger people. We have lots of phone calls already, people wanting to ask about vaccinations. So tell us about the process that the FDA and the CDC followed to decide Pfizer’s mRNA vaccine was a good fit for kids under 12.
ANGELA RASMUSSEN: Right. So this is a great question because a lot of people have been wondering about it. They’ve been wondering why we approved vaccines for 12 to 15-year-olds a while back and now we’ve approved it for 5 to 11-year-olds. And some people want to know when we’re going to be approving it for kids even younger than that. And that’s because every time you approve a vaccine for younger age groups, you have to do a clinical trial.
And the clinical trials in this case were done in what’s called an age de-escalation trial scheme. So that basically means that you start with the older kids. You enroll them in the trial. You make sure that they’re not seeing any severe adverse events that weren’t seen in adults. And then you progressively enroll younger and younger age groups.
So that’s why the clinical trial that was enrolling the 5 to 11-year-olds finished up about a month and a half ago. And that data was then submitted to the FDA for consideration and approval. And then, of course, the ACIP, the Advisory Committee for Immunization Practices, also examined that data and made recommendations. And now that vaccine is authorized and available for 5 to 11-year-olds.
That trial enrolled about 3,000, or a little over 3,000 kids. It was primarily looking at both safety and efficacy. But one of the challenges in doing clinical trials in groups like those 5 to 11-year-olds who are low risk for developing symptomatic COVID-19 is that it is very difficult to look at efficacy the same way that you would do that in an adult group where people are at high risk.
So they weren’t necessarily looking as much at COVID infections, although there were some in the trial and it certainly did appear that the vaccines reduced symptomatic COVID-19. But they’re also going to be looking at the immune responses that it provokes as well as the adverse event profile and safety profile.
And what they found was that, yes, the vaccine was efficacious at preventing symptomatic COVID-19 in kids. It also induced robust immune responses that are thought to be protective similar to the adults who developed these immune responses, such as neutralizing antibodies. So we expect that it will be very effective at population scale. And importantly, I think a lot of parents want to hear this– there weren’t severe adverse events reported.
That said, though, we really don’t have the ability to identify rare events even in much larger clinical trials. So the one in a million, one in 500,000 type events are normally during the vaccine clinical trial process for any age group identified usually once those vaccines come out onto the market. But in general, parents, I think, should be relieved that this virus has– or this vaccine– sorry, not the virus– the vaccine has an excellent safety and efficacy profile in those 5 to 11-year-olds. So people can feel confident getting it.
IRA FLATOW: We have some excellent questions from excellent listeners, too. So let’s see if we can get them on. First, let’s go to Belinda in Arizona. Hi, Belinda.
BELINDA: Hello.
IRA FLATOW: Hi, there. Go ahead.
BELINDA: So I have an 11-year-old boy– actually, two of them– twins. And I was concerned a little bit about the reaction that some of the 17-year-olds had around heart pain. And I wanted to know if any of the trial’s kiddos had that. And if so, what is the rate, I guess? And then what other specific side effects had you seen in the trials?
IRA FLATOW: Thanks for that question. Angela?
ANGELA RASMUSSEN: Yeah, that’s a fantastic question and it’s one I’ve been getting a lot. People are certainly worried about the risk of myocarditis that could be in younger kids since it does seem to be associated with the older younger people, and especially younger boys or men have had this myocarditis. And the good news there is that nothing was seen in the trial because it’s an extremely rare adverse event. So it really doesn’t happen.
Hundreds of thousands, millions of these doses have been given to 12-year-olds and up. There have only been a few hundred cases of this myocarditis. And what people should really think about, too, is that these cases of myocarditis, even when they’ve resulted in hospitalization, have been very treatable. So these are transient self-limiting cases of myocarditis when they do happen. And then when they do, they are extremely rare.
But that said, as I was mentioning before, this trial was too small to actually detect those cases because they happen at such an infrequent rate. So it is something that we should be looking out for and we should be making sure that we do have a good understanding of what that rate is in the real world.
IRA FLATOW: All right, let me get a phone call or two before the break. Let’s go to Erin in Clearwater, Kansas. Hi. Hi, Erin.
ERIN: Hi. Wonderful to speak with you.
IRA FLATOW: Nice to have you. Go ahead.
ERIN: Thank you. I, too, have twin boys, which is a fun coincidence. I have two eight-year-olds and a five-year-old, and we were waiting on pins and needles for the vaccine to come out. And last Tuesday they got COVID. So I’m wondering what your recommendation is for when they can get the vaccine or when it’s safer-wise to get all my three kiddos the vaccine now that they have had COVID.
IRA FLATOW: Good question. Thanks for calling.
ERIN: Thank you.
ANGELA RASMUSSEN: That’s a fantastic question, Erin. And I think a lot of people have really been wondering this. If my kids had COVID, why do they even need to get the vaccine? And the answer to that is that kids don’t have the same response to having COVID all the time as far as their immune system is concerned. So there’s a lot of variability.
It doesn’t sound like you need to be convinced to actually get your kids vaccinated once they’ve recovered. And I hope that their recovery is very swift and that they don’t have a lot of lasting problems from it. But in general, you want to make sure that you’ve waited a while after their recovery to get a vaccine. And the reason for that is that when they were infected, your immune system will still respond to SARS-coronavirus-2. It will mount immune responses. And then it will take a little bit of time to settle down.
When they get their first vaccine shot, the immune system is basically going to say, oh, I remember you, SARS-coronavirus-2 spike and respond accordingly. That will help lock in those really potent protective neutralizing antibody responses that hopefully will last for a long time. So I would ultimately consult your kid’s pediatrician or provider on what the actual length of time should be. But it should be at minimum probably two to three weeks and potentially even a little bit longer after they’ve recovered before you go and sign them up for their first shot. But I’m delighted to hear that you’re going to.
IRA FLATOW: It’s amazing how many people are calling about kids– the vaccine now that they can get it. It seems like there’s great interest in it.
ANGELA RASMUSSEN: Which is really wonderful to hear. I’ve seen lines stretching down the block in a number of places in the US with people just really, really enthusiastic about getting their kids vaccinated. And that’s wonderful to see.
IRA FLATOW: Well, we’re going to have to take a break. Let me give out the number again. Our number is 844-724-8255. If you’d like to call to Dr– talk with Dr. Angela Rasmussen about kids and vaccines. We have lots of callers on the line, but we have lots of room for more callers. So we’re happy to see our first day back in the studio with Science Friday that our listeners are still there and they are all interested in still calling in. We’re happy to have you. 844-724-8255. More with Dr. Angela Rasmussen after this break. Stay with us.
This is Science Friday. I’m Ira Flatow. In case you’re just joining us, we’re doing Fact Check My Feed. Yeah, your feed about the virus and the vaccines with Dr. Angela Rasmussen, a research scientist at VIDO-InterVac. That’s at the University of Saskatchewan. And our number 844-724-8255. So many people. So many calls. Let’s see where– let’s go to this line. Let’s go to Pittsburgh. Chris, hi in Pittsburgh. Welcome to Science Friday.
CHRIS: Hi. Thank you. I understand that the mRNA vaccine causes your body to produce the spike protein and that it can pass through the blood brain barrier and go into the ovaries. Does anybody know what the long-term effects of that will be?
ANGELA RASMUSSEN: Yeah, that is a great question, Chris. And I would say that for the most part, we don’t know the long-term effects of that. But these vaccines have been given to women now for people who can get pregnant– people with ovaries– for over a year. And we have seen no impacts on reproductive health during that time. That to me suggests that the long-term impact of potential entry of the spike protein into the ovaries is really incidental and that there’s no ill health effects.
IRA FLATOW: Let’s go to Tanya in Colorado. Hi, Tanya.
TANYA: Hi, how are you today?
IRA FLATOW: Fine. How are you?
TANYA: I’m good. I just wanted to ask a question. I’m actually a pediatrician and have been for the past 25 years and have given probably thousands of vaccinations. And what concerns me about what your guest is suggesting is that children do not have the same immune response that adults have to the COVID vaccine. And as much as I’d like to believe that, as a physician, I’d like to understand where that information came from since we’re not– we haven’t been giving vaccines to children.
And how was it determined that children do not have the same ability to mount a satisfactory immune response as they do to the multitude of vaccinations that they’re given as children? And as an older adult, I can tell you that I still have immunity to the measles, mumps, and rubella. So that’s my question is, where is this data coming from and how are they obtaining it to make this statement?
IRA FLATOW: All right, thanks for your question. Angela?
ANGELA RASMUSSEN: Yeah, I’m glad to have the opportunity to clarify, because actually that’s not what I’m saying at all. I think what I was– what may have been misunderstood was when I said that because in the clinical trial it’s really much more difficult to assess efficacy in a population that’s low risk of developing symptomatic disease, which is the endpoint for that trial. To actually do that based on COVID cases, you have to look at immune responses.
And in this case, they were looking specifically at neutralizing antibody responses and Th1 responses. And what they found was that vaccinated kids in this age group had very similar responses to adults. So it actually– that’s really the opposite of, I think, what you understood me to say is that these vaccines are actually provoking very similar responses to what would be provoked in adults.
And they probably need a lower dose, because, actually, as you pointed out, too, immune protection and robust immunity declines with age. So these kids have really potent, very young healthy immune systems, and they’re responding to this virus by generating neutralizing antibodies that effectively render the virus non-infectious to the same levels or actually even a little greater than adults do.
IRA FLATOW: Mhm. Twitter question from John who asks, what about children under five? Why is nobody talking about when they will be able to receive a vaccine? Asking for my two-year-old son.
ANGELA RASMUSSEN: Well, people are definitely talking about this. And I have the same question for my own two-year-old, almost three-year-old niece. And the correct answer to this is that we don’t really know, but it’ll probably be sometime early next year. Because as I mentioned, this is an age de-escalation trial. So the last groups to be fully enrolled in the trial and tested and monitored over the trial period are going to be those younger groups of kids.
So as soon as we can get enough kids enrolled in the trial and get enough data from them to provide the FDA with enough data for them to make an evaluation, that will happen. And I think that probably a realistic timescale is January or February of 2022.
IRA FLATOW: Speaking of data, what goes into figuring out the dosage level for vaccines when kids are involved?
ANGELA RASMUSSEN: So this is also a complicated question that is a little bit different given the expedited clinical trial process. And usually, one of the reasons the clinical trial process takes so long is that there is a fair amount of dose optimization that occurs during that trial for all different age groups. In this case, we needed to get vaccines out onto the market and into people’s arms as quickly as possible. So it was really relying on pre-clinical work and work from the early phase one, phase two clinical trials to decide these doses.
Given that it does appear that dose is somewhat associated with severe adverse events, and given that there has been this observed, although rare, risk of myocarditis, a decision was made to use a lower dose for these younger kids. Also, because, as I was mentioning for the prior caller, these kids do have really robust immune systems that respond very well, so they may not need a larger dose– the same dose that older people do need.
IRA FLATOW: All right, still lots more questions on the phones. Let me close my eyes and just throw a dart here. Let’s go to James in Kentucky. Hi, James.
JAMES: Ah.
IRA FLATOW: Hi, go ahead.
JAMES: Hello, Ira. My daughter is eight years old. We’ve had her– she’s had the flu vaccine several years ago and she had an adverse reaction to that. How does that predict with her taking the COVID vaccine?
IRA FLATOW: All right, thank you.
ANGELA RASMUSSEN: That’s a great question, James. And this is one of those where I unfortunately have to cop out and tell you to talk to your pediatrician for your daughter, because it really depends on what type of severe adverse event that was, what type of flu vaccine she had it to. So many flu vaccines are grown in eggs. That’s not an issue with these vaccines. But for some people who are allergic to eggs or who have an issue with tolerating egg proteins, they can’t take those egg-derived flu vaccines.
If it’s something like that, then the COVID vaccine may be no problem. If it was something more serious, like anaphylactic shock, to vaccines in general, that would probably recommend her– against her getting vaccinated. So this is really something I would encourage all parents, if you have any concerns about your child’s vaccination history, to talk with your provider prior to getting them vaccinated, because you definitely don’t want to be giving a vaccine to somebody who is going to have a severe adverse event because of it.
IRA FLATOW: Let’s go to Cincinnati. Emily in Cincinnati, hi. Welcome to Science Friday.
EMILY: Hi. Thank you. Happy birthday.
IRA FLATOW: Thank you.
EMILY: I’m calling as the mother of a 17-year-old and a few months who has type 1 diabetes, who has had two Pfizer vaccinations. The second one was in April. And so my question is about boosting the kids who are fully vaccinated and moving beyond that six-month window that we hear is so important. And especially with a child with an autoimmune disorder, waiting until July next summer is going to be a long wait.
IRA FLATOW: Yeah.
EMILY: So thank you.
IRA FLATOW: Yeah. Thank you, Emily. So what do you think about that?
ANGELA RASMUSSEN: So again, this is going to be a situation for the caller’s son specifically to talk to their provider about it. But in general, I would say that boosters are not harmful. Boosters are really an issue in terms of vaccine supply. The reason why we’re not recommending boosters for everybody right now is because we actually still have quite a few unvaccinated people, believe it or not, who need to get those vaccines as well.
But for somebody with type 1 diabetes of any age, that is a risk factor for severe COVID. I would say that person is certainly eligible for a booster shot and should be able to get one.
IRA FLATOW: I want to break away from our main topic of discussion to talk about one thing that is really fascinating and maybe alarming story this week. Something I think your research connects to. And that is deer in Iowa that seem to be getting COVID-19 from us and transmitting it to each other. And in one study, almost 80% of deer– 80% were infected. What’s going on there, Angela?
ANGELA RASMUSSEN: Yeah, so I’m really glad you asked about this, Ira, because it does indeed coincide with my work. I’m leading a project within the Coronavirus Variants Rapid Response Network, which is a Canadian research network here, looking into this. And really what that points to is that there is significant risk for what we call spill-back.
So spillover is when a virus that’s circulating in wild animals spills over zoonotically to the human population. This is where the virus has spilled back into a population of animals. And we’ve already seen spill-back occurring in other species. Most notably, in Denmark and the Netherlands, this occurred with minks. We also see it happening with big cats in zoos and all of these zoo animals that we’ve heard about getting infected. Dogs and cats as well– companion animals.
So spill-back is a real risk, not necessarily to those deer. I haven’t seen anything at least that suggests that this is wiping out the deer. But it is a risk when you have animals that are in frequent contact with people, as deer are, and live in very populated areas, that the virus starts spreading in the deer. Potentially new deer-specific variants can emerge that could also potentially infect humans. And that could be a real problem, both in terms of vaccine efficacy as well as potentially it could be causing more severe disease in humans or have at least unpredictable properties.
Now, this isn’t something that people should lay awake thinking about are the pandemics never going to end. We’ve known this is a risk for a long time. But I think more than anything this should be a wake-up call that we really do need to understand that we’re not the only species affected here. And really controlling COVID is much more than just controlling it in the human population. We also need to be surveilling wildlife and looking for animal reservoirs before they do become a problem in terms of spill-back creating new animal reservoirs for this virus.
IRA FLATOW: You know that’s what my next question was– the spill-back and the deer as reservoir. The big question is whether they’d be able to transmit the virus back to us. That’s what people probably are most worried about.
ANGELA RASMUSSEN: I think so. I mean, I think that they should be because of the way that we would interact with deer. And I think there’s been a lot of confusion about this because people have said, well, deer live outside. I thought this was transmitted by aerosols. Yes, that’s true among people. But it may be different with deer.
And so the way that we interact with those animals is going to be really important. For example, is a hunter who comes into contact with a deer that they have– that they’re preparing as wild game– is that going to put them at increased risk? Are people just encountering deer in the wild going to increase their risk? Is activities like feeding deer, petting deer, if they’ll let you– and some deer will– a lot of them are afraid of people.
But we need to think about how we interact with these animals and interact with the natural world to really better understand the risk of cross-species transmission. And if not deer, there are a number of other species. This virus is a very generalist virus. This virus has infected many, many cats. And we all know that when we have pet animals– it actually can infect dogs, too– a lot of times with our pets, we’re very affectionate. We touch them a lot. We let them lick us. We give them kisses.
These are all activities that potentially could put people at risk. So we really do need to be figuring out which animals are getting infected, identifying when they are infected, and potentially treating them or developing vaccines for them, because there is significant risk whenever we interact with wild animals that there could be cross-species transmission.
IRA FLATOW: It’s good news to hear that we’re following them or should be following them. I’m Ira Flatow. This is Science Friday from WNYC Studios. Talking with Dr. Angela Rasmussen. Our number 844-724-8255. Let’s see if we can get a few more calls in before the break. Let’s go to Jake in Kansas. Hi, Jake. How are you? Jake, are you there?
JAKE: Hey!
IRA FLATOW: Hey!
JAKE: Good afternoon, guys. Hey! I appreciate you taking my call.
IRA FLATOW: Go ahead.
JAKE: So I have an 11-year-old daughter who’s getting her HPV shot next Tuesday. We just scheduled her COVID shot for Friday. I know there is no interactions with the flu shot, but has there been anything with any of the other shots?
IRA FLATOW: HPV and other shots, Angela.
ANGELA RASMUSSEN: Not that I’m aware of. And generally, vaccines don’t interact with each other at all. And the reason for that– I mean, this is why kids tend to get a lot of vaccines, especially when they’re really young and they’re just getting their childhood immunizations. That’s why it’s not a problem to immunize them against many things at once.
The immune system responds to each vaccine very specifically. So you’re not going to have a lot of cross-talk, or any cross-talk really, between a flu vaccine and the SARS-2 vaccine, or an HPV vaccine and a SARS-coronavirus-2 vaccine. And even if you did, probably the only impact would be that it would boost immunity to both of those vaccines.
So you can rest assured that you’re definitely doing the right thing in immunizing your daughter against HPV. There was just a huge study that came out that showed that it has dramatically cut the incidence of cervical cancer. So that’s wonderful. And protecting her against SARS-coronavirus-2 is wonderful as well. Rest assured you’re doing the right thing.
IRA FLATOW: Let me see if I can get this last question in quickly. Because we know the holidays are coming up and kids who get vaccinated right now won’t be fully vaccinated by that time, right? Thanksgiving is going to roll around. There are still kids under five and their families are thinking about it. Are this year’s holidays any different in terms of safety from last year’s?
ANGELA RASMUSSEN: I think they are because for one thing we have a lot more adults who are vaccinated. And I think that depending on the type of holiday gathering you’re going to have, there are measures that you can put in place to make it safer for everybody, including unvaccinated or partially vaccinated kids. One of those things is to limit the size of the gathering or to limit it only to relatives that you know are adults who– or older kids– who have been vaccinated fully already.
Another thing that people could start implementing– and they’re not yet available as widely as they should be. They’re not going to be within everybody’s pricing range. But applying rapid tests is something that you can do as well before your Thanksgiving gathering to make sure that everybody who’s coming there is not going to be infected or contagious with SARS-coronavirus-2. So I think we have more tools than we had last year. I don’t think there needs to be a blanket ban on holiday get-togethers, even if there’s a couple partially vaccinated kids around.
IRA FLATOW: But if you’re a grandparent of a very young child and you still feel uncomfortable about gathering this year, you say still don’t go if you don’t feel comfortable being there.
ANGELA RASMUSSEN: I mean, I think that applies any time. If you don’t feel comfortable or if the boundaries that are being set for a particular gathering you’re not comfortable with, then don’t go. But really last year I didn’t get together with my family, even though they lived across town, for both Thanksgiving and Christmas. And this year I will be traveling back for Thanksgiving, even though I have this unvaccinated two-year-old niece, because all of the adults are vaccinated and all of the older adults have gotten booster shots.
IRA FLATOW: So make a wise decision, but think about it. And it’s safer this year than last year.
ANGELA RASMUSSEN: It’s safer this year than last year. And especially think about the different layers of protection that you can put in place. We’re going to do rapid tests if we can get those, too.
IRA FLATOW: All right, we’ve run out of time. And as always, thank you for taking time to be with us today, Dr. Angela Rasmussen, research scientist at VIDO-InterVac, the University of Saskatchewan’s Vaccine Research Institute in Saskatoon, Saskatchewan. Thank you, Angela. It’s always a pleasure to have you.
ANGELA RASMUSSEN: My pleasure, Ira. And it’s so good to be back on with you live.
IRA FLATOW: Thank you. We have to take a break. And when we come back, it’s a big milestone in making cows greener. Think about it. It has to do with what they burp. We’ll talk about the whole thing. It’s a follow-up we talked about earlier. We’re going to see how it’s working out. Stay with us. We’ll be right back after this short break.
Copyright © 2021 Science Friday Initiative. All rights reserved. Science Friday transcripts are produced on a tight deadline by 3Play Media. Fidelity to the original aired/published audio or video file might vary, and text might be updated or amended in the future. For the authoritative record of Science Friday’s programming, please visit the original aired/published recording. For terms of use and more information, visit our policies pages at http://www.sciencefriday.com/about/policies/
Christie Taylor was a producer for Science Friday. Her days involved diligent research, too many phone calls for an introvert, and asking scientists if they have any audio of that narwhal heartbeat.
Ira Flatow is the founder and host of Science Friday. His green thumb has revived many an office plant at death’s door.