‘Breakthrough’ In Sudden Infant Death Syndrome Research Is Misleading
11:53 minutes
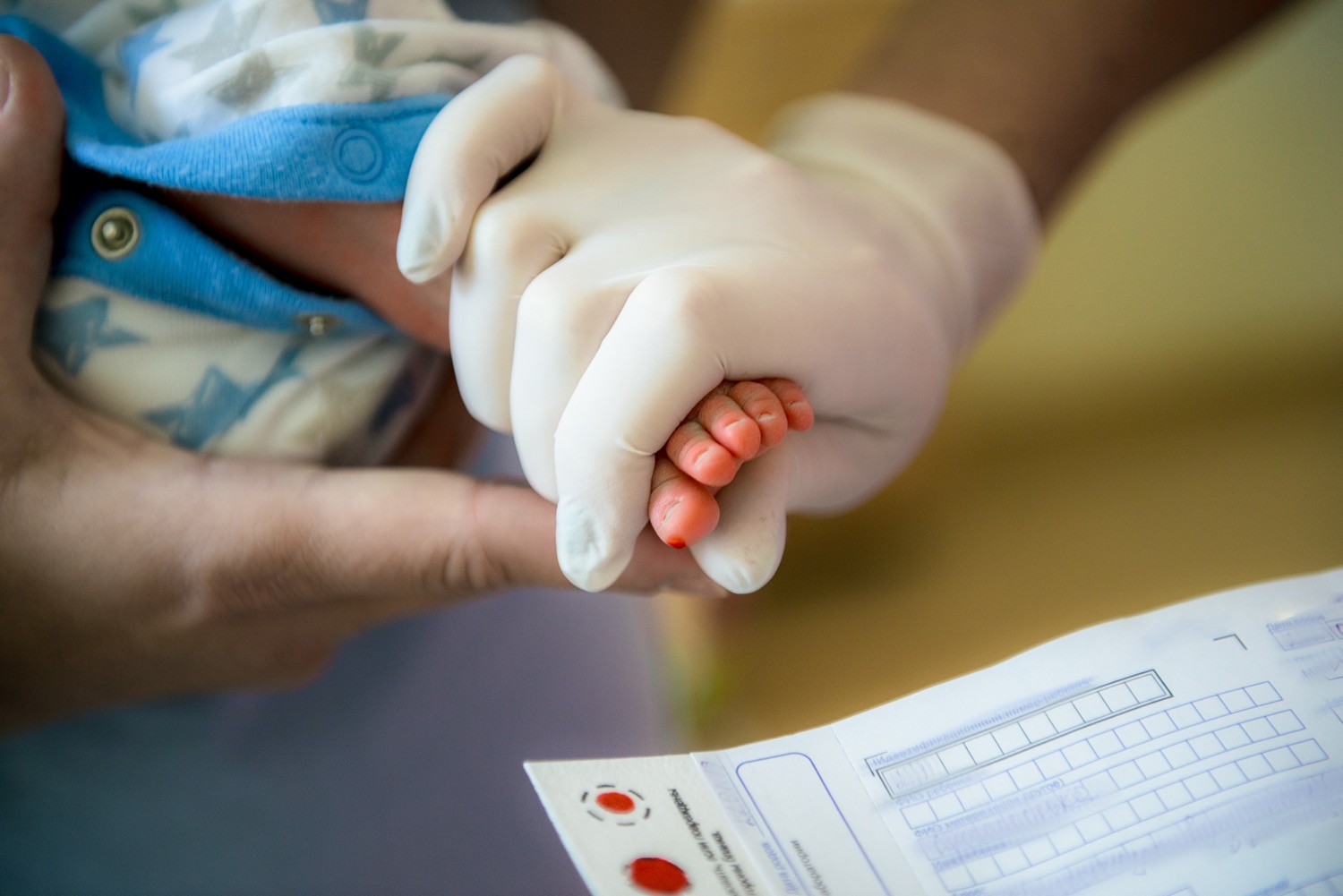
Last week, headlines made the rounds in online publications and social media that there was a massive breakthrough in research about SIDS: Sudden Infant Death Syndrome. A study out of Australia concluded that babies who died of SIDS had significantly lower levels of an enzyme called BChE. This study was met with cheers by people desperate to understand why SIDS happens.
But many experts say we need to pump the brakes on the celebration. While the study may be promising, it was based on a very limited sample—just 26 babies who had died of SIDS. A variety of factors could explain their different levels of BChE, says Dr. Rachel Moon, a professor of pediatrics and SIDS research at the University of Virginia.
Moon explains that there are two major hurdles for researchers trying to investigate the causes of SIDS. First, as grieving parents are very unlikely to consent to their deceased child’s use in medical studies, the sample pool for genetic testing of SIDS death is incredibly small. Secondly, there are just very few people who specialize in the syndrome; Dr. Moon suspects there are one hundred or fewer researchers of SIDS in the entire world.
Dr. Moon joins guest host John Dankosky to discuss how these factors make it hard for researchers to study why some babies continue to die prematurely.
Invest in quality science journalism by making a donation to Science Friday.
Rachel Moon is a professor of Pediatrics and a SIDS researcher at the University of Virginia School of Medicine in Charlottesville, Virginia.
JOHN DANKOSKY: This is Science Friday. I’m John Dankosky. Ira Flatow is away. If you follow children’s health, you may have seen the headlines last week– reports of a big breakthrough in research about SIDS, Sudden Infant Death Syndrome. About 3,500 babies die suddenly and unexpectedly each year in the US.
A study out of Australia found that babies who died of SIDS had significantly lower levels of an enzyme called BChE. Now, this study, of course, was met with cheers by people who are desperate to better understand why SIDS happens. But some experts are saying we’ve got to pump the brakes on the celebration. SIDS is a devastating situation for parents, and the truth is, there’s a lot we don’t know about it. While the study is promising, there’s more we still need to learn.
So joining us here for a reality check on the state of SIDS research is my guest, Dr. Rachel Moon, professor of pediatrics and SIDS researcher at the University of Virginia School of Medicine. She’s also chair of the American Academy of Pediatrics Task Force on SIDS. Welcome to Science Friday, Dr. Moon.
RACHEL MOON: Thank you for having me. It’s great to be here.
JOHN DANKOSKY: First, why don’t you tell us a bit about this study that came out of Australia. What exactly did it suggest?
RACHEL MOON: This study looked at dried blood spots of babies who had died from SIDS, babies who had died from another cause, and control babies. And what they found was that the serum levels of one enzyme called butyrylcholinesterase was statistically lower in the babies who had died of SIDS. And so this created a huge media and social media flurry.
JOHN DANKOSKY: It did create quite a flurry. These headlines were saying things like, this is the breakthrough in SIDS we’ve been waiting for. We’ll have a cure for SIDS. So what’s the reality here? What was your take on this paper?
RACHEL MOON: So I think it’s an interesting paper. It’s a very preliminary result. There were only 26 babies who had died of SIDS who were represented in this study. And even though the levels were statistically lower in those babies, there was a great deal of overlap. So at this point, I don’t think that we can use this as a biomarker, because if you get one level, you can’t make a prediction about whether or not a baby is at higher risk or not because there’s just too much overlap.
However, it does remind us that there are neurotransmitters in some babies where there is deficiency or some kind of difference in how the neurotransmitters work, and that there is, for many of these babies, some kind of biological predisposition. And then when that baby is placed in a situation where they are experiencing some asphyxia– so that means a lower level of oxygen or a higher level of carbon dioxide– that they may not arouse, and they may not wake up to be able to respond appropriately to that stimulus. And so it does remind us that it’s not just one thing that causes SIDS, but it’s probably a perfect storm of several events happening at once.
JOHN DANKOSKY: Yeah. In a minute, I want to talk a little bit more about the research that you do and the other research that is out there right now. I guess I should ask, though– people did get very excited about this research. In your mind, what caused this excitement? I mean, why were so many people in the media, even in the science media, picking up on this story and saying, oh my goodness, we may have a breakthrough here?
RACHEL MOON: You know, that is a very good question. I think those of us that are working in this area were a little bit surprised at how quickly this gained momentum. And none of us predicted this. I think that there are several reasons.
It’s such a devastating disease. Even though we know more about it than we did 20 or 30 years ago, there’s still a lot of mystery left. There are a lot of grieving parents out there, people who have lost their babies before. And they’re still left with this answer of why.
And many of them have experienced stigma, because a lot of people– there’s this perception out there that SIDS only happens to people who are bad parents, and it can’t happen to me because I’m a good parent. And so then when it does happen to you, then you’re treated differently by other people. And so to be able to say, it wasn’t anything that I did, but it was something that was innate in my baby, that is really very hopeful for people.
And so I think that there is a lot of hope. There’s a lot of fear. There’s also a lot of– there are a lot of people who don’t want to follow the safe sleep guidelines because they’re hard. They’re hard to follow. And so if we have a blood test that can diagnose it, then we can do away with all of that.
JOHN DANKOSKY: Well, let’s talk about those safe sleep guidelines and some of the work that you do seemingly on the completely other end of the spectrum here, not having to do with finding specific biomarkers of what may cause this in babies, but really just applying best practices as far as we know them right now in order to keep kids as safe as possible. What can you tell us about these safe sleep practices?
RACHEL MOON: Well, these are pretty much tried and true. I mean, it’s not 100%, but they do reduce your risk significantly. So these are things like, place your baby on a back in a crib or a bassinet or a place that is flat and with a firm surface. And there should be nothing but the baby in that sleep environment.
Breastfeeding is protective. Being in a non-smoking environment, that is also protective. And using a pacifier is actually protective as well. So those are the mainstays of the safe sleep guidance that we provide to families.
JOHN DANKOSKY: And we know that these things work. But as you say, it’s not 100% foolproof.
RACHEL MOON: That’s right. You know, so once back sleeping was recommended, the rates of SIDS declined by 50% in the US and in most places around the world that also recommended this. But since 2000, we have not seen a change in the rate of SIDS. It has not gone down. And these deaths still continue to happen.
Part of it is because of unsafe sleep practices, or at least that is contributory. Part of it is also that these babies, many of them have an innate inability to wake up. There’s something going on in their brainstem. And there’s been a lot of work done on brainstems and neurotransmitters and arousal. And these babies can’t wake up. And so it’s this combination of things that contribute to these deaths.
JOHN DANKOSKY: So what is the status of research on SIDS right now? When it comes to biomarkers of the type that we’re talking about from this Australian study, neurotransmitters, the inability of babies to wake up, what’s the scope of the research being done right now in the world on SIDS, doctor?
RACHEL MOON: There is a lot of work being done on the brainstem and looking at neurotransmitters. There’s a lot of work being done at Boston Children’s by Hannah Kinney and Robin Haynes. And there’s work being done all over the world on this.
I say all over the world, and it makes it sound like there are a lot of us doing it. There actually are not that many people doing research in this area. We’re a very small community.
And so we believe that what happens is that these babies ultimately can’t wake up when they need to wake up. And this is likely because there’s some kind of break in the neurotransmitter connections. There’s been a lot of attention on serotonin. There’s also been a lot of attention on acetylcholine. These are a couple of the neurotransmitters that there’s been a lot of focus on and there have been some differences in.
In terms of biomarkers, something that you could test for, we actually were hopeful a few years ago because there were some promising signs that looking at serum blood levels of serotonin might be helpful in identifying which babies might have an arousal defect or be at higher risk for these deaths. But the latest that I heard, which was earlier this month, it looks like that is not the case, at least not right now.
So at this point, I mean, we’re closer than we were 10 years ago. But I would not say that there’s going to be a biomarker in three to five years. So what we’re left with is doing the things that we know will reduce the risks. And those are the safe sleep practices.
JOHN DANKOSKY: And it’s hard to find these biomarkers because of the difficulty in finding tissue samples.
RACHEL MOON: It is very difficult to find tissue samples. So as I mentioned, and as everybody realizes, when your baby dies, it’s the worst thing in the world that can happen to you. And so you’ve lost your baby. The police are coming to talk to you because they have to investigate this sudden and unexpected death.
And so you feel like you’re already being stigmatized. There’s all of this emotional thing happening to you. And then somebody tells you that they’re doing an autopsy, which is routine for these babies, and they ask you if you want to donate samples that can be saved for research. And you are probably not in the right mind to be able to do that because of all of the stuff that’s happening to you that you are overwhelmed with.
In every state except for one, parental consent is required before tissue samples can be gotten. And in California, which is the one state that does not require parental consent, most medical examiners are very reluctant to get tissue samples without parental consent. And that’s certainly understandable.
So it’s very, very difficult to get tissue samples. And it’s interesting because if you talk to parents later on, they many times wish that they had said yes and they had given consent. But at that moment in time, they just couldn’t do it. It was just too much for them.
JOHN DANKOSKY: You know, obviously, 3,500 deaths, or more than that depending on the diagnosis, is a huge number of cases. But even beyond that, every parent in the world who fears for their child’s safety and tries to follow safe sleep practices is concerned every day about this happening. This is, doctor, just such a huge issue. And I guess it just shocks me when you say that there’s not that many people like yourself studying this around the world.
RACHEL MOON: It shocks me, too. So number one, the media doesn’t cover this. And number two, the rates did go down after the Back to Sleep campaign. And so there’s this perception that this is a disease that has gone away.
And so it’s very difficult to get funding to study this. It’s very difficult to find junior people who want to study this, because it’s hard to get funding. And so it becomes this vicious, vicious cycle.
But I don’t even think there are a hundred people of us around the world that are doing this work. And that includes the pathologists, the biochemists, the geneticists, the epidemiologists, the physiologists, all of these people. I don’t even know if there are a hundred of us around the world.
JOHN DANKOSKY: That’s all the time we have. I’d like to thank our guest. Dr. Rachel Moon is professor of pediatrics and a SIDS researcher at the University of Virginia School of Medicine. She’s also chair of the American Academy of Pediatrics Task Force on SIDS.
RACHEL MOON: Thank you so much for having me.
JOHN DANKOSKY: We’ve got to take a break. When we come back, we’re looking into how period-tracking apps store and share your data and the role of digital privacy in a post Roe v. Wade era. Stay with us.
This is Science Friday from WNYC Studios.
Copyright © 2022 Science Friday Initiative. All rights reserved. Science Friday transcripts are produced on a tight deadline by 3Play Media. Fidelity to the original aired/published audio or video file might vary, and text might be updated or amended in the future. For the authoritative record of Science Friday’s programming, please visit the original aired/published recording. For terms of use and more information, visit our policies pages at http://www.sciencefriday.com/about/policies/
Kathleen Davis is a producer and fill-in host at Science Friday, which means she spends her weeks researching, writing, editing, and sometimes talking into a microphone. She’s always eager to talk about freshwater lakes and Coney Island diners.
John Dankosky works with the radio team to create our weekly show, and is helping to build our State of Science Reporting Network. He’s also been a long-time guest host on Science Friday. He and his wife have three cats, thousands of bees, and a yoga studio in the sleepy Northwest hills of Connecticut.