Zika Virus Transmission Still Mysterious
9:57 minutes
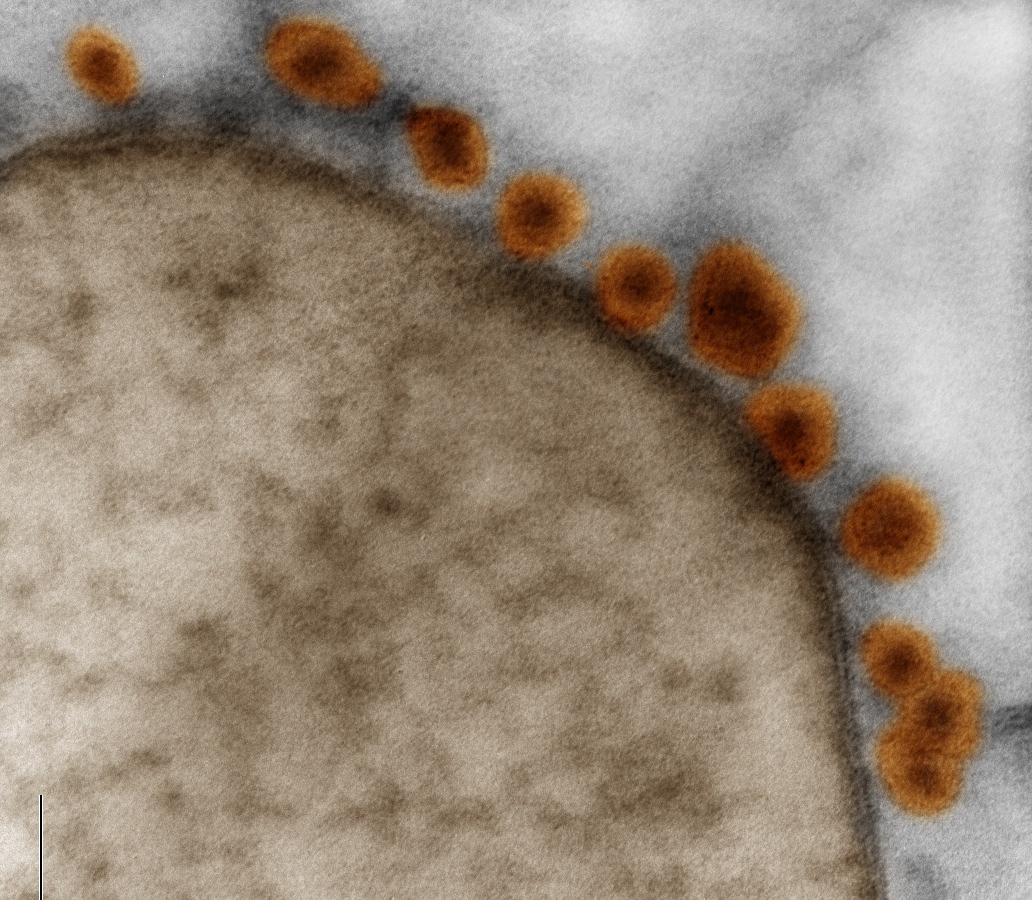
This week the CDC announced that there’s finally enough evidence to draw a definitive connection between Zika virus and microcephaly, the condition where infants are born with unusually small heads and brain damage. But many questions remain, such as how the virus passes from mother to child. Microbiologist Carolyn Coyne explains.
Carolyn Coyne is an associate professor of Microbiology and Molecular Genetics at the University of Pittsburgh in Pittsburgh, Pennsylvania.
IRA FLATOW: This is Science Friday, I’m Ira Flatow. This week, the Centers for Disease Control and Prevention announced that there’s finally enough evidence to draw a definitive link between Zika virus and microcephaly. That is the condition where infants are born with unusually small heads and brain damage. Here is CDC Principal Deputy Director, Anne Schuchat.
ANNE SCHUCHAT: Everything we look at with this virus seems to be a bit scarier than we initially thought. And so while we absolutely hope we don’t see widespread local transmission in the continental US, we need the states to be ready for that.
IRA FLATOW: Are the states ready, though? Are we prepared to diagnose Zika in mothers here in the US? Can we determine whether their unborn babies have been affected? And with closing of so many clinics in the South, where can women infected with Zika virus turn to end a pregnancy they fear might result in a deformed child?
Also, there are Zika mysteries remaining, like the one my next guest has been studying. And that is, how does the virus even pass from mother to child. Carolyn Coyne is an associate professor of microbiology and molecular genetics at the University of Pittsburgh in Pennsylvania. She joins us from WQED. Welcome to Science Friday.
CAROLYN COYNE: Hi, thank you for having me.
IRA FLATOW: You’re welcome. Dr. Coyne, one of the things that I just mentioned that you’ve studied is how the virus might pass from the placenta, from mother to fetus, which is sort of a rare thing among viruses, isn’t it?
CAROLYN COYNE: Oh, absolutely. You know, overall we know very little about how all viruses, even those associated with congenital disease, pass from mother to fetus. But I think in general the thinking is that actually very few viruses are actually capable of doing that. And so there is something quite unique, I would say, about Zika, that somehow has afforded it the ability to do that.
IRA FLATOW: Do you have any clues about how that might be happening?
CAROLYN COYNE: Well I think right now we’re still in the process of trying to establish even the model systems by which to test this. Because pregnancy represents, I think, a bit of a unique scientific, at least model, system, by which to study this. Because the human placenta changes dramatically throughout gestation. And so the placenta that is in a woman in the first trimester is actually very distinct from the placenta in the second and third trimester.
And so some of our work so far has, I think, directly pointed to a mechanism of vertical transmission of the virus that does not involve the actual replication of the virus in the placenta cells themselves, which are called the trophoblast cells, at least in the second half of pregnancy. But it does not mean that that does not happen in earlier stages of gestation, let’s say in the first trimester.
IRA FLATOW: Now that the virus is beginning to appear in the US, mostly in the South so far, do we have a quick way of diagnosing it in a lot of people?
CAROLYN COYNE: Well, I think that’s going to be the trick. Because certainly we can look for– the easiest way, I think, to diagnose this, of course, will be based upon symptoms in the pregnant woman– fever, rash, those kinds of things. And then, of course, after that, you can look for the presence of the virus or potentially antibodies, of course, in the maternal blood.
Diagnosing though whether that infection has resulted in congenital Zika syndrome, I think will be a little bit more difficult. Because depending upon the stage of pregnancy, depending upon the severity of the disease– such as microcephaly, but now we know that there are actually other congenital syndromes associated with Zika– could actually be very difficult to diagnose.
IRA FLATOW: But the virus has been around a long time. And we’ve known about it for a long time. Why would we only be seeing these birth defects now?
CAROLYN COYNE: Well, that’s, I think, the big question. That’s sort of the million dollar question. And so as a virologist, I think you look at things like is it the virus that’s changed? Is it the host that has changed? Or potentially is it both?
And I think we don’t know enough yet, to really be able to pinpoint if it is not one or some component of all of those factors. We know, certainly, that the virus itself has changed. So the sequence of the virus that was first circulating in Africa is quite distinct than the virus that’s circulating in Brazil right now.
But we also, though, could say that there may be something very different about the women in Brazil, so therefore the host, that has somehow allowed them to become, and their babies therefore, much more sensitive to Zika virus. I’d say right now we have some just hypotheses and ideas, but we really don’t have direct data.
IRA FLATOW: Could it have something to do with timing? You know, when the infection happens?
CAROLYN COYNE: It could potentially. I don’t think it explains why that wouldn’t have happened in other outbreaks that have occurred, certainly in more recent years throughout the world. I think certainly the microcephaly that we’re seeing in a lot of these fetuses is likely to result from probably first trimester, early pregnancy infection, simply because that is, of course, at the stage when neuronal development is most active, and the developing fetus is most sensitive to anything that, of course, disrupts that process.
But we should keep in mind, though, that other pathogens and other viruses that are associated with congenital disease actually can cause microcephaly. So this is not something that is special to Zika. Toxoplasma gondii, rubella, cytomegalovirus, herpes virus in some cases. These viruses, as well as toxo, can also induce microcephaly.
IRA FLATOW: There are only about 20 abortion clinics left in Texas. There’s one for all of Mississippi. Are we potentially facing a situation where only the well-off, people who can afford to travel to get an abortion to end their pregnancy, if they suspect their baby might be infected with the Zika virus.
CAROLYN COYNE: I think we absolutely could be. And I think that’s one of the issues that I think has been largely overlooked when thinking about the fact that we now have the mosquito, or very soon we’ll certainly have the mosquito vector that could certainly transmit Zika to Americans in the southern United States very, very soon, if not of course right now. And so I think those kinds of questions we have to start having an open dialogue about. That if women in early pregnancy in the United States are confirmed to have a Zika infection, as I mentioned before, it may actually be very difficult to diagnose any congenital disease in those developing fetuses for several months in pregnancy.
And if those women then make the decision to opt for an elective abortion, how will they do that? Will they be able to do that? Where can they go? And I think that that’s a very, very important question.
IRA FLATOW: Another abortion related issue your following is a Tennessee representative, Marsha Blackburn, and her effort to subpoena the names of any researchers even tangentially involved in fetal tissue research. She wants to create a public list. Is that going to put a chill on fetal tissue research, potentially important to Zika related research?
CAROLYN COYNE: I would say absolutely. I think those kinds of things are terrifying, I mean, certainly to scientists. But also to keep in mind that the list that is being curated involves not just the list of the principal investigators but the members of our laboratories who are doing that work. So students– young students– technicians, postdoctoral fellows, what have you.
So I think it’s going to scare, certainly, the investigators who are leading these studies. But I think extending that list to the people in the lab doing the research is really quite frightening. It certainly is frightening to the members of my lab and to the labs of collaborators of mine that work in fetal tissue.
IRA FLATOW: But you know, it’s interesting that this issue has come right into the teeth of the political system. Right now, we’re–
CAROLYN COYNE: That’s exactly right.
IRA FLATOW: You know? You think this might be not just a national issue but a local issue as well?
CAROLYN COYNE: I think it should be an issue that we’re all thinking about, certainly in terms of the political landscape. But also that we really, I think, just as a society, even beyond just the politics, really have to start thinking about these kinds of things related to reproductive health, women’s rights. And certainly with something like Zika, I think it’s at least perhaps more quickly moved into the forefront of our dialogue.
IRA FLATOW: So what do you tell women in general who are fearful about getting the Zika virus?
CAROLYN COYNE: Well unfortunately, I don’t think there’s much we can say. And again, that’s sort of the disappointing and scary thing about it at this stage of the outbreak, because we really know so little about that.
And certainly, I’m asked routinely, as someone who at least studies the more reproductive angle of the vertical transmission, should I have a baby, when should I have a baby. And the issue is we just know so very little about this. We still don’t know, as I mentioned before, whether it is something unique in the host, so the Brazilian women that are somehow allowing the virus to undergo this vertical transmission that would not happen in the United States.
And I think fairly soon, we should begin to see whether there actually is a congenital Zika disorder associated with infection in American women. And if it’s not, then I think that that points us in some directions, I think very obvious and important directions, as to what could be different about women in Brazil.
IRA FLATOW: Right. And who would be studying that?
CAROLYN COYNE: I think we’re all– I mean, I think a lot of us are studying it. Certainly the virologists are studying it, those of us that are interested in vertical transmission of viruses– interested in how the placenta, which is this really unique organ in human biology protects the developing fetus. So I think we’re all really trying to, as quickly as possible, assemble groups together, to start asking these questions.
IRA FLATOW: Well, I want to thank you for taking time to be with us today. We’re going to certainly watch this. And as you say and as you point out, this political season will be very interesting.
I think this is going to be raised, as we get into the summer, and we see possibly more cases of the Zika virus. People are going to start asking about what we do about this. And hopefully our politicians will have some answers.
CAROLYN COYNE: Absolutely. And I hope people do ask. And I hope people ask very loudly and very forcefully.
IRA FLATOW: Carolyn Coyne is an associate professor of microbiology and molecular genetics at the University of Pittsburgh in Pennsylvania. Thank you very much Dr. Coyne, for taking time to be with us today.
CAROLYN COYNE: Thank you for having me.
Copyright © 2016 Science Friday Initiative. All rights reserved. Science Friday transcripts are produced on a tight deadline by 3Play Media. Fidelity to the original aired/published audio or video file might vary, and text might be updated or amended in the future. For the authoritative record of ScienceFriday’s programming, please visit the original aired/published recording. For terms of use and more information, visit our policies pages at http://www.sciencefriday.com/about/policies.
Christopher Intagliata was Science Friday’s senior producer. He once served as a prop in an optical illusion and speaks passable Ira Flatowese.