Are Probiotics Good For You? Not Always
16:54 minutes
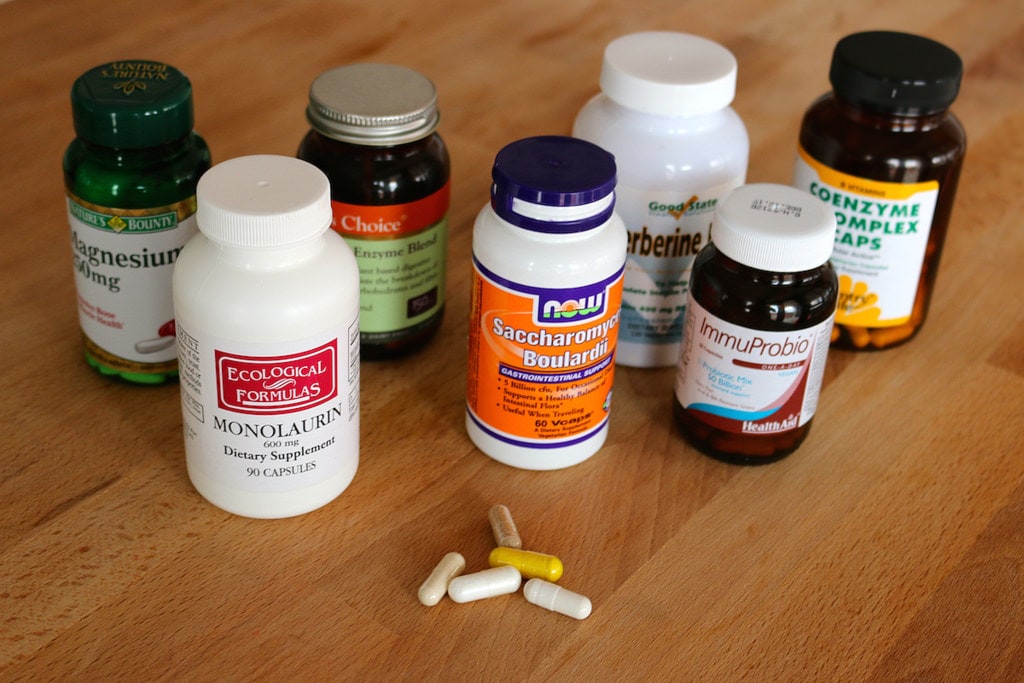
Are probiotics good for you? The answer to that question seems baked right into their name: pro-biotics. We’ve all heard about the benefits of a healthy gut microbiome. Probiotics are one way we try to give our digestive system an extra dose of that good bacteria.
Studies have shown that probiotics can help prematurely-born babies fight intestinal inflammation. And perhaps they can help older women from developing weaker bones. But what about everyone else? Can popping a few probiotic supplements do any harm?
[This anthropologist’s lab filled with ancient teeth might just be a tooth fairy’s fantasy.]
The answer is yes. Too much of any bacteria, even the good kind, can be harmful to your digestive system. And if probiotic supplements headed for your colon dump their contents too early, bacteria in your small intestine can cause symptoms of brain fogginess. Dr. Satish Rao, Professor of Medicine at Augusta University, joins Ira to discuss why we should proceed with caution when it comes to probiotics.
What do probiotics do?
Probiotics are live bacteria that can help replenish the community of microorganisms living in the colon. In theory, probiotics are supposed to aid those who have digestive disorders and bowel inflammation.
What are these supplemental probiotics doing?
Supplemental probiotics should be dumping live bacteria in the colon, which is part of the large intestine. Ideally, the pills should stay intact as they go through the small intestine, but a recent study from Dr. Satish Rao, Professor of Medicine at Augusta University proved that wasn’t the case. Instead, the pills were releasing their contents in the small intestine, causing brain fogginess, gas, and bloating in a majority of the patients—in fact, some of them quit their jobs. And as Rao said, there are “hundreds and hundreds of [probiotic supplements] out there with virtually no studies on them.” These, and most other supplements, are not regulated in the same way that food and traditional drugs are.
Are there any probiotic supplements on the market that release their contents in the large intestine?
None, according to Rao. “[Pills] would be a fantastic way of taking probiotics so that they exclusively deliver this product in the colon. But I don’t think there’s any methodology that I’m aware of that can guarantee that, which I think is the unfortunate problem.”
If someone has been taking probiotics for awhile, should be they be worried?
The good news is that the body has an array of defense mechanisms. The small intestine is a very active part of the body. “It secretes about six to ten liters of fluid a day,” said Rao. Most of the time, that acid flushes the small intestine and keeps it sterile.
“But there are various things that may mess it up,” said Rao. “If you take too much probiotics and if your gut is slow or you don’t have much acid, then you have set a potential stage where the bacteria can colonize [the small intestine].”
What about fermented foods that have natural probiotics?
Instead of probiotic supplements, Rao recommends fermented foods like yogurt and kefir that have natural probiotics. The amount of probiotics in those foods is “not as much as what is packaged in the probiotic capsules.” Plus, Rao says, there are food ingredients that make the live cultures less potent.“I believe that the natural probiotic foods are safe and good. And I would encourage everybody to take it.”
Satish Rao is a professor of Medicine and Director of the Digestive Health Clinical Research Center at Augusta University in Augusta, Georgia.
IRA FLATOW: This is Science Friday. I’m Ira Flatow. Have you ever wonder whether probiotics are good for you? I take probiotics. I think they’re good for me. Maybe I have to rethink some of this stuff, because there’s new research coming out all the time on probiotics. And we’re going to talk about some of it now.
Of course, the name probiotics itself, right? The name seems baked right in, into their name. Probiotics– pro– they must be good for you. We’ve all heard about the benefits of a healthy microbiome. And probiotics are one way we try to give our digestive systems an extra dose of that good bacteria.
But what do we really know about them? What do we really know so much about the microbiome itself? We know that studies have shown that probiotics can help preemie babies fight intestinal inflammation. Other studies suggest they can help older people from developing weaker bones. But what about everyone else? Even if we can’t yet quantify the benefit, popping a few probiotics can’t do any harm, right?
Well, in fact, my next guest says the opposite could be true. Too much of any bacteria, even the good kind, can be harmful to your digestive system. And if probiotic supplements headed for your colon dump their contents too early, bacteria in your small intestine can cause symptoms of brain fogginess, he says. So is it time to throw those probiotics into the trash? Not so fast. Dr. Satish Rao is professor of medicine and Director of the Digestive Health Clinic Research Center at Augusta University. Welcome to Science Friday.
SATISH RAO: Thank you, Ira.
IRA FLATOW: I want to give out our phone number– 844-724-8255. Folks might be very interested in talking about that. Also you can tweet us @scifri. So you know, most people who are familiar with probiotics– but for those who aren’t, give us a small definition of what they are and why would somebody want to take one?
SATISH RAO: So the WHO has defined probiotics as live micro organisms that confer health benefit if ingested in sufficient quantities. Now, that is the WHO your definition. So in simple terms, these are bacteria that hopefully will replenish our colonic microflora and give us health benefit.
IRA FLATOW: So when the probiotic is working properly, the bacteria should go into your large intestine, your colon area.
SATISH RAO: That is correct. Now, we have, what, about 500 billion bacteria and about 500 different species of bacteria in the colon. So it’s a very large population of bacteria and different species. But most probiotic formula that we have available now, they probably have anything between two to 10 or 12 different types of bacteria. That’s all we have in the probiotic group.
IRA FLATOW: Now you say that the bacteria can go wrong, things can go wrong with them. We don’t want them in our small intestine, our upper GI tract.
SATISH RAO: That’s correct. So they’re designed or at least believed to– once we ingest it in a capsule form, they’ll go unchanged through the stomach, through the small bowel, and get into the colon and confer their health benefits. But that has not been very categorically and systematically proven. There is very little data to say that if you take a particular probiotic– and then they’ve collected poop, if you like, at the other end to see whether they are really culturing these bacteria coming out at the other end. Now, there are some– very few studies. But the majority don’t. And we have hundreds and hundreds of preparations out there with virtually no studies on them.
IRA FLATOW: So they’re not regulated at all, as if they were a drug. People are taking them thinking they’re maybe like an herbal medication.
SATISH RAO: That’s how most people are taking it. Most people believe that it confers health benefits, just like taking a multi-vitamin pill. And it is not a multi-vitamin pill. They are live bacteria that we are taking. And for the majority of folks, I suppose it doesn’t do a lot. But for some, it can cause significant harm. And that’s what we found in our study.
IRA FLATOW: Tell us about what you found.
SATISH RAO: So I, as a gastroenterologist, usually see patients with belly problems. So they come to me with belly pain, gas, bloating, distention, sometimes constipation, diarrhea. These are common problems. So I’ve been seeing these kind of patients for 20, 30 years of my career.
But in the last five to seven years, we suddenly started seeing patients who are, in addition to these symptoms, reporting brain fogginess. Now, that’s a rare symptom for gastroenterologists. I guess if you have brain fogginess, you may see your internist. You may see a neurologist or a psychiatrist but not a gastroenterologist. But these folks were really coming with this unusual symptom in addition to their belly problems.
So we said this is odd. Why are these guys having brain fogginess? So we really set about to try and find out what is going on. Our initial hypothesis was that they were producing something in their gut that was getting absorbed into the body and somehow causing fogginess in the brain.
And now we do see some patients– for example, we see patients with chronic liver disease. These are people with liver failure or kidney failure, who do have some fogginess. And that’s because of accumulation of ammonia or urea and so on. But this was very odd. We said these folks don’t have liver failure. They don’t have kidney failure. Yet they were foggy.
So we then decided to start looking at a number of potential products that they may be producing in the body. And then we found that these folks or a majority of them were producing large amounts of D-lactic acid. And this D-lactic acid, normally we produce very little amount in the body. Mostly we produce L-lactic acid, which is the lactic acid that we all produce now. When we run or jog we get cramps. And that cramps is because of lactic acid, L-lactic acid accumulation.
But only very small amounts of D-lactic acid is produced in the body, mostly in the gut, whereas these folks were producing large amounts, largely because of fermentation of sugary foods in the small bowel. And it was this excessive accumulation of D-lactic acid that was causing the brain fogginess.
IRA FLATOW: Wow. And that was because the probiotics were hanging out in the small intestine instead of being where they were supposed to be.
SATISH RAO: That is correct. So normally, as I said, we see patients with bacterial overgrowth. And these bacteria usually don’t produce D-lactic acid. When they ferment sugars, they produce hydrogen, methane, and other gases. But they usually don’t produce much D-lactic acid or very small amounts.
But if your gut is colonized, your small bowel is colonized with probiotic-containing bacteria, such as lactic acid or [INAUDIBLE] such as Lactobacillus or Bifidobacterium, which is commonly present in most probiotics, then you have a different population of the small bowel, which now has the capacity or the ability to ferment the sugars and in addition to producing hydrogen, methane, and other gases, also produce D-lactic acid. That is what was happening in these patients.
IRA FLATOW: And you could see it actually happening in the patients?
SATISH RAO: We could because what we did was we brought the patients into a lab. And then we gave them glucose as a drink, which is a standard drink we give as part of a glucose breath test, a test we use for detecting Small Intestinal Bacteria Overgrowth, or SIBO. So we gave them this drink. But before they consumed the drink, we measured their blood and urine lactic acid levels.
And we gave the drink. And then after the drink, at one, two, and three hours, we once again measured their blood and urine lactic acid along with their breath samples. And we found that in a significant, almost 70% of these patients who were presenting with brain fogginess, there was a significant elevation or increase in lactic acid production.
IRA FLATOW: Wow. That’s quite interesting. So should you prescribe– I mean, people– I’m looking at my phone bank here. Some people are on the way to the drugstore in their cars. They’re saying what probiotic should I get? I mean, or should I not? Am I wasting my time? And is it a question of not getting the probiotic or is it a question of making sure it stays encapsulated in the delivery system until it gets to your large intestine?
SATISH RAO: Well, I think if somebody can guarantee that, I guess that would be a fantastic way of taking probiotics so that they exclusively deliver this product in the colon. But I don’t think there’s any methodology that I’m aware of that can guarantee that, which I think is the unfortunate problem. So they can break down anywhere.
But fortunately, most of us have various defense mechanisms. Acid is a good defense mechanism in the stomach. The small bowel has fantastic motility. It is the most active organ in the entire gut. And it is bathed by acid. And it secretes about 6 to 10 liters of fluid a day. So all of those tend to flush the small bowel and keep it sterile most of the time.
But there are various things that may mess it up. If you take too much of probiotics and if your gut is slow, you don’t have much acid, or your motility is problematic, then you have set a potential stage where the bacteria can colonize the small bowel.
IRA FLATOW: Let me go to the phones to [? Alaina ?] in Ventura, California. Hi. Welcome.
[? ALAINA: ?] Hi. I was calling to see what your guest thinks about the probiotics found in kombucha and other fermented foods.
IRA FLATOW: Yeah, good question. Yogurt, whatever.
SATISH RAO: So that’s a very good question. The amount of probiotics in fermented foods, particularly yogurt or kefir and so on is not as much as what is packaged in the probiotic capsules. Plus, you take a lot of other materials along with the food. So I believe that the natural probiotic foods are safe and good. And I would encourage everybody to take it. They’re probably good. But the way we are taking it, perhaps, with the form of capsules with billions and billions of bacteria may not be the best for everybody.
IRA FLATOW: What percentage of your patients do you think who take probiotics come down with these symptoms?
SATISH RAO: I think it’s– what we are seeing is just a tip of the iceberg, is what I believe you’re seeing. I’m sure there are millions out there who have this problem but they have either not consulted or the doctors have not made the association. I’m sure there are a lot of folks with this. But I don’t want to say that probiotics is all bad. It is good. I prescribe probiotics as well.
I give it in highly selective conditions. There are patients in whom the gut flora has been damaged, altered, disturbed, particularly diarrheal situations, people who have taken antibiotics, people in whom they’ve had long diarrheal illness, where the colon bacteria have been flushed out. In those situations, it is appropriate to take it. But to take it for any GI disorder just because you have some pain, you’ve got some gas, you’ve got some bloating or constipation and expecting these probiotics to really work miracles, I think is not the right way to move forward. And there is very, very, very little science to support it either.
IRA FLATOW: I’m Ira Flatow. This is Science Friday from WNYC Studios. Talking about probiotics with Dr. Satish Rao, professor of medicine at Augusta University. Let’s go to the phones to Joy in San Jose. Hi, Joy.
JOY: Hi. Thank you for taking the call. I have a question that’s a little bit different. I had my colon removed over 30 years ago. And I have been taking probiotics, because I thought it would be good for me to get some of those bacteria back in my system. But now you say it’s bad in the small intestine. So I’m a little concerned that– I haven’t had any mental confusion or any of that, but I’m just curious if this is not something I should be doing.
IRA FLATOW: Good question.
SATISH RAO: Yeah, I think that’s a very good question. I would be cautious about taking probiotics if you don’t have a colon. In fact, we’ve seen a lot of patients– a paper that we reported earlier this year are patients like yourself who have had colon removed who have a very high predisposition for SIBO, Small Intestine Bacterial Overgrowth.
And in fact, many of these patients are presenting recurrent to the hospital with gas and bloating and distention because they either have a small rectum, a small part of the colon that is left behind, which now has a long passage or a clear connection to the small bowel and bacteria from within that small, one-foot rectum is now constantly contaminating the small bowel, and they’re getting SIBO. So I think it is a problem there. However, if you’re getting benefit from taking probiotics, maybe I would let you let you carry on with it.
IRA FLATOW: 30 years– there’s a long track record.
SATISH RAO: Absolutely.
IRA FLATOW: Well, one question we talk about, what I wanted to ask you, because we did a research story the other day on Archaea. It’s not quite a bacteria. It’s a form of life, the third form of life. And we heard it populates in a lot of different places. And I was wondering, do we have archaea in our gut of our own? Are there trillions of them in there?
SATISH RAO: Yes, Ira. I listened to your program. I was very fascinated and educated a lot from that program as well. But it’s an area that we’ve been researching for the last 10, 15 years. We do have archaea in the gut. And we have a few– one of them is methanobrevibacter smithii. There is a methanobrevibacter oralis, which is in the mouth. And smithii is one of the big archaea which is in the gut, predominantly in the colon.
And what is interesting is we found this association between this archaea, methanobrevibacter smithii that tends to produce a lot of methane and constipation. It almost seems like a fingerprint for constipation, this particular archaea that seems to exist in the colon. And we’ve seen that patients who have more refractory, more difficult-to-treat constipation produce large amounts of methane. And also they have IBS-like symptoms. So both IBS, constipation, and chronic constipation seems to be associated with this. It is not to say that everybody with constipation has this archaea. But those who have archaea, they seem to have the more challenging, more difficult-to-treat constipation.
IRA FLATOW: So it’s the archaea that’s producing the gas in our gut?
SATISH RAO: They are. So the archaea have– this methanobrevibacter, for example, has a unique ability to take in carbon dioxide, as your guest was saying last time, and hydrogen, and convert that into methane. So we don’t know evolutionary why we’ve acquired this archaea, but they must– they probably do play an important role. One of the roles probably is to reduce the amount of gas production in the body. I’m sure that is an important role they play. But whether at some stage, they actually cause problems like constipation, I think that is our area of inquiry right now.
And I really do believe that it actually causes constipation. We’ve gone on to do one study where we have tried to decrease this archaea by giving antibiotics. And we had some marginal success. I wouldn’t say we had great success. But we had some marginal success. And we are now just in the early stages of a clinical trial, where we are using a novel statin in– the same statins that people take for cholesterol lowering. There is one form of statin that seems to have an interesting role in inhibiting an enzyme that leads to archaea reproduction. And we are in the early stages of this to see whether this particular statin compound may decrease this archaea and thereby lead to resolution of these challenging constipation symptoms.
IRA FLATOW: Well, we love to follow the microbiome, so we’ll be following your research, doctor. Thank you very much for taking the time to be with us today. Dr. Satish Rao, professor of medicine, director of the Digestive Health Clinic Research Center at Augusta University.
Copyright © 2018 Science Friday Initiative. All rights reserved. Science Friday transcripts are produced on a tight deadline by 3Play Media. Fidelity to the original aired/published audio or video file might vary, and text might be updated or amended in the future. For the authoritative record of Science Friday’s programming, please visit the original aired/published recording. For terms of use and more information, visit our policies pages at http://www.sciencefriday.com/about/policies/
Katie Feather is a former SciFri producer and the proud mother of two cats, Charleigh and Sadie.