Wireless Monitoring Gives Parents Greater Access To Newborns In The NICU
7:49 minutes
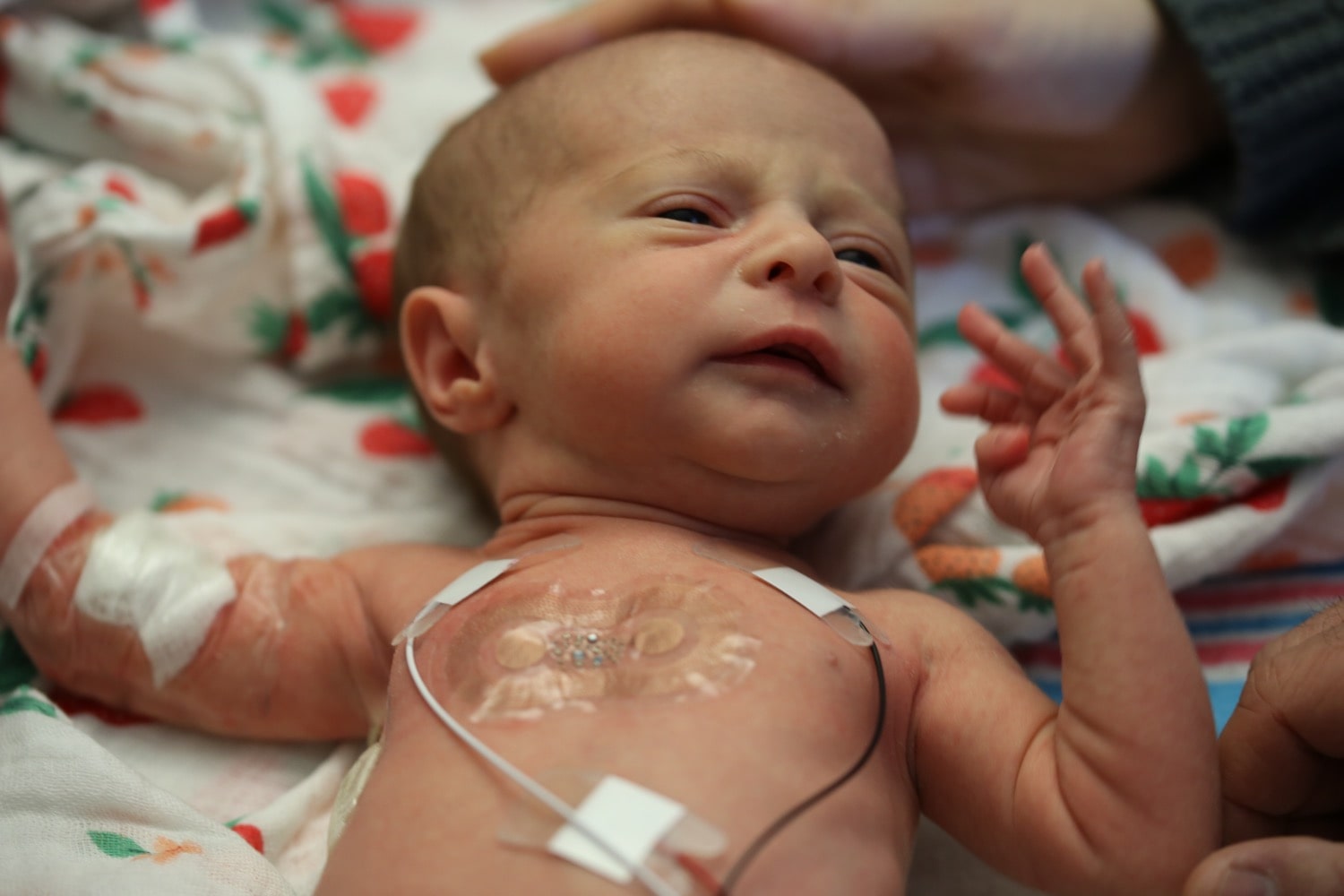
What’s more terrifying than becoming a new parent? Starting out as new parents in the Newborn Intensive Care Unit, where babies spend their first days entangled in wires attached to sensors that monitor their vital signs. Most of the time, parents can only helplessly look into the crib and see what looks more like a science experiment than a kid.
But in the digital age, why must wires and sensors take up so much real estate on a tiny baby? That’s the question driving the development of a new monitoring device—a small wireless sensor that takes the scary “science experiment” effect out of the NICU, and gives parents more time to cuddle with their newborn.
John Rogers, professor of Material Science and Engineering and director of the Center for Biointegrated Electronics at Northwestern University, joins Ira to discuss how the new device could transform neonatal care in the U.S. and in developing nations around the world.
John Rogers is a professor of Material Science and Engineering and director of the Center for Biointegrated Electronics at Northwestern University in Evanston, Illinois.
IRA FLATOW: What’s more terrifying than becoming a new parent? Well, finding your newborn in the neonatal ICU, all tangled in wires attached to sensors that monitor his or her vital signs. And most of the time, parents can only helplessly look into the crib, see what looks more like a science experiment than a kid. But in this digital age, why must wires and sensors take up so much real estate on a tiny baby?
That’s the question driving the development of a new monitoring device, a small, wireless sensor that takes the scary science experiment effect out of the NICU and gives parents more time to cuddle with their newborn. Joining me to tell us more is John Rogers, professor of material science and engineering, and director of the Center for Bio-Integrated Electronics at Northwestern University. Welcome to Science Friday.
JOHN ROGERS: Yeah, hello. Hey, thanks for having me.
IRA FLATOW: That is a scary sight, is it not, when you see a newborn?
JOHN ROGERS: Well it’s pretty daunting. I mean, I don’t have any personal experience with that, but we work with parents of premature babies all the time. And it’s pretty easy to see the kind of experience that they’re going through. And so our hope here is to, through advances in engineering science, sort of change that situation and make it a little bit more humane for the babies, the parents, the nurses, the neonatologists, and allow things to be done in a different way.
IRA FLATOW: So you have a wireless sensor that is recording the heartbeat, the body temperature, the blood flow, transmitting it to where?
JOHN ROGERS: It transmits it to an external data recording device. And so we can send it to a smartphone or a tablet, or a laptop computer or a desktop system, anything that’s equipped with Bluetooth wireless functionality.
IRA FLATOW: And so then mom or dad, or any of the doctors or nurses can come in and actually pick up and cuddle the baby because it has no wires attached to it.
JOHN ROGERS: Yeah. I mean, I think that’s one of several advantages of the technology, relative to the old way of doing things. The other is that the hard-wired devices demand rather strong adhesive tapes to keep them in good contact with the skin of the baby. But the problem is these premature babies have very underdeveloped skin. It’s very mechanically fragile. Those tapes have to be removed on a 24-hour cycle to clean and maintain the baby.
And that peel back process oftentimes leads to skin injuries, peeling of the skin. And this is a fairly frequent occurrence. And so by eliminating those strong adhesive tapes and the wires, replacing that kind of approach with a soft, skin-like, lightweight sensor that can just gently adhere to the surface of the skin, you really eliminate that risk. So there’s a whole series of benefits of this technology over the clinical standard that’s out there today.
IRA FLATOW: This is Science Friday from WNYC Studios. I’m Ira Flatow talking with John Rogers. OK, so what was the hardest thing to get right about these wireless sensors?
JOHN ROGERS: Well, there’s a lot of hard things, I guess. I mean, if you can think about these devices as a skin-like type of platform– it’s radically different than what you see in consumer gadgetry today. So your smartphone is a great piece of technology, but it’s rigid. It’s inflexible. It’s hard. It’s totally incompatible with soft tissues of the human body, the skin being one example.
So we really had to reformulate electronics into an entirely different form factor, one that adopts the thickness, the mechanical properties, the bending rigidity of the skin itself to allow this gentle conformal interface to this very fragile surface so that that skin contact can be used as a window for measuring underlying body processes. So I think that the form factor was a challenge. The other thing that kind of flows from that is a device that’s sort of paper thin and has this kind of mechanics. Can’t be powered in the usual way. You can’t plug in a AA battery. I mean, it just completely destroys the mechanics.
You have to think about ways to drive power efficiency of the computational resources that are available on these devices and the radio frequency communication links that allow us to stream the data, do all that in a very power-efficient way. And we are actually able to operate these devices battery free. So we actually use a wireless power transfer scheme to deliver the operational power to the platforms, use that same link to pull data back out. So there were some challenges in that sense as well.
I would say the third is that it’s not actually a single device. It’s a pair of devices, one that goes on the chest. The other one goes on the foot. And they operate in a time-coordinated fashion to reproduce all of the clinical-grade accuracy that’s supported by these hard-wired, taped on sensors in this much less invasive, skin-like wireless platform.
IRA FLATOW: Is it possible now then for the baby to go home still wirelessly wired?
JOHN ROGERS: Well, we think so. If you take a look at the parents, I mean, they’re certainly nervous with their babies in this kind of science experiment, as you describe it, with all the wires and so on. It turns out that they get even more nervous when they think about taking the baby home and removing it from all of that monitoring equipment. And I think these kinds of technologies would very naturally translate to the home setting so that the monitoring could continue and the attending physicians, the nurses, the neonatologists could have access to that data, thereby extending sort of the NICU level of monitoring into a home setting. And I think there’ll be a lot of value there.
IRA FLATOW: Is it possible yet to do that? I mean, take it home and hook up to your home Wi-Fi, still monitor?
JOHN ROGERS: Well, yeah, we are able to do that now. And so this paper represents a state of the art for us. About four to six months ago was just the cadence of how scientific publication works. And so in the meantime, we’ve sort of adapted these platforms to align with manufacturing practice in sort of cutting edge consumer electronics technology.
And the goal there is to deploy these devices into the developing world. So almost like a home setting, certainly much different than the level for NICU that we’re operating in at Lurie Children’s Hospital, downtown Chicago. So with partnerships and funding from the Gates Foundation and the Save the Children Foundation, we will be deploying tens of thousands of these units into the developing world, starting with Zambia in April, extending to India, Pakistan, and Kenya by the end of the year.
IRA FLATOW: So you’ll have a sort of double duty for these, third-world countries and also right here.
JOHN ROGERS: Well, we think so. So we’re looking to expand the deployment here domestically, but I think the developing world is a fruitful area as well because there aren’t monitoring technologies that need to be displaced. There’s just nothing there right now. And so being able to deliver that information is going to be very, very powerful.
If you look at the rates of mortality and the rates of premature births, they’re highest in the developing world. So I think there’s a tremendous need and opportunity here that also is enabled by the relatively low cost structure associated with these platforms, certainly compared to the high-end monitoring equipment that exists in hospitals here in the US. And so there are a lot of things that are driving it.
IRA FLATOW: Well, we wish you good luck, professor. And thank you for taking time to be with us today.
JOHN ROGERS: Yeah, thank you for having me.
IRA FLATOW: John Rogers, professor of material science and engineering at Northwestern University.
Copyright © 2019 Science Friday Initiative. All rights reserved. Science Friday transcripts are produced on a tight deadline by 3Play Media. Fidelity to the original aired/published audio or video file might vary, and text might be updated or amended in the future. For the authoritative record of Science Friday’s programming, please visit the original aired/published recording. For terms of use and more information, visit our policies pages at http://www.sciencefriday.com/about/policies/
Katie Feather is a former SciFri producer and the proud mother of two cats, Charleigh and Sadie.
Ira Flatow is the founder and host of Science Friday. His green thumb has revived many an office plant at death’s door.