Why Are Children’s Antibiotics So Hard To Find Right Now?
8:06 minutes

This article is part of The State of Science, a series featuring science stories from public radio stations across the United States. This story, by Farah Yousry, was originally published by Side Effects, from WFYI Public Media.
Mary Warlo has been extremely worried lately.
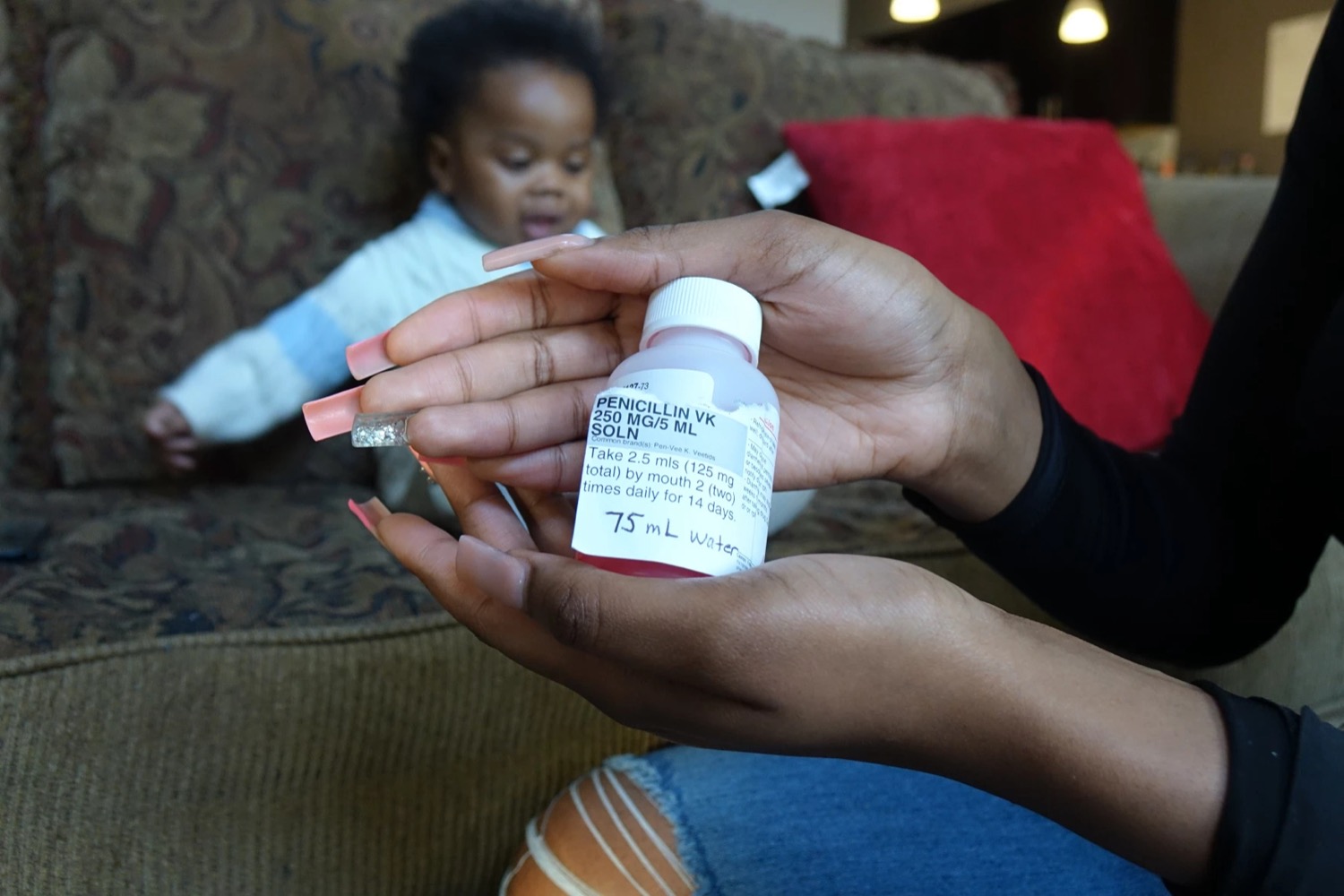
Her baby Calieb, who is six months old, has sickle cell disease. In early December he went for a few days without liquid penicillin, a medication that he—and thousands of other children in the U.S.—rely on to prevent potentially life threatening infections.
Warlo couldn’t easily find a pharmacy in Indianapolis that had the medicine in stock. She and her husband frantically drove around for hours, stopping at five different pharmacies before they were able to get their prescription filled.
“It was extremely stressful and I am worried about what will happen the next time we need to fill his prescription two weeks from now,” she said.
Pediatric sickle cell disease specialists say they are alarmed by signs that the stock of liquid penicillin is dwindling in some places. They say children’s lives depend on this medication, and a penicillin shortage could spell disaster.
“I’m most worried that all of the work that we’ve done over the decades to ensure that our infants and children with sickle cell disease can live long and healthy lives will be compromised, because of them not being able to access… a basic medication,” said Dr. Seethal Jacob, a pediatric hematologist who treats sickle cell disease at Riley Children’s Hospital in Indianapolis.
Every year, 2,000 babies are born in the U.S. with sickle cell disease, a complex genetic disorder that affects the blood. The vast majority of sickle cell patients are Black.
As recently as the early ‘80s, nearly 1 in 3 children with sickle cell disease would die before their fifth birthday. Then, a landmark clinical trial found that a simple intervention could slash rates of life-threatening bacterial infections by more than 84 percent. The intervention involved two doses of preventative penicillin, administered daily between 2 months and at least 5 years of age.
Thanks to the widespread use of penicillin—and mandatory newborn screening for sickle cell disease—the death rate for children with sickle cell disease has plummeted over the past several decades. Today, more than 95 percent of children with sickle cell disease born will reach their 18th birthday.

Sickle cell disease weakens the immune system of children who have it, which makes a bacterial infection extremely risky.
Jacob is worried that more of her patients will end up in the hospital with serious bacterial infections and said that she is “significantly concerned that some of them may become so ill that they would pass from that infection as well, or its associated complications.”
The U.S. Food and Drug Administration tracks drug shortages and has not indicated that there is shortage of penicillin in the U.S.
But some hospitals like Riley Children’s in Indiana—and also St. Louis Children’s Hospital in Missouri—notified providers in early December that their liquid penicillin stock is running low, advising them to look for other alternatives.
Warlo said her doctor told her that if she can’t get liquid penicillin for her son Calieb, they may have to switch him to penicillin tablets. Warlo would need to crush the tablets and put them in his feedings.
One alternative to penicillin for children with sickle cell disease is an antibiotic called amoxicillin. Dr. Monica Hulbert, a pediatric sickle cell specialist at St. Louis Children’s Hospital, said she prescribed it to one of her patients the week of Dec. 1, but they were unable to find it in stock because of an ongoing nationwide shortage of amoxicillin.
Hulbert said the penicillin shortage is likely to push providers to prescribe alternative antibiotics with a broader range of coverage than penicillin, which can be a lot more expensive for patients. Some alternative antibiotics may also require prior authorization from insurance—a process that could take anywhere from 48 hours to a few weeks, Hulbert said, leaving children with sickle cell vulnerable to potentially life-threatening infections.
Hulbert also worries that as shortages for some antibiotics persist, there could be a ripple effect.
“The trick is that when one thing is unavailable, then everybody switches to the next thing. And then, demand may exceed supply on that too,” Hulbert said.
Antibiotic shortages in the U.S. are common, said Erin Fox, a senior pharmacy director at the University of Utah.
Fox has been tracking antibiotic shortages since 2001 and has found that antibiotics are always present among the top five drugs in short supply every year—and that could be for several reasons.
“These are older drugs, they’re generic drugs, they are low-cost drugs. And so because of those characteristics, there’s actually not a lot of incentive for manufacturers to have any extra on hand or any kind of backup supplies,” Fox said.
During the current shortage some manufacturers said they’ve been hit by labor shortages, Fox said. She’s also been hearing from more manufacturers who say that they’ve been holding their end of the contract, producing the amount of antibiotics they have been asked to produce.
But it seems that this year, that’s not enough, said Michael Ganio, senior director of pharmacy practice and quality at the American Society of Health-System Pharmacists.
Ganio said the current shortage doesn’t appear to be due to manufacturing hiccups or quality issues. It’s more likely a shortage driven by a sharp increase in demand over the past several weeks.
The country is dealing with a surge in infectious diseases “after a period of latency due to COVID-related mitigations like masking, remote work and schooling and social distancing,” he said.
Ganio is worried that the current shortage might have ripple effects—a shortage of one drug can fuel the shortage of alternatives for that drug.
“This is unusual, in that we’re seeing the second and third choices affected,” Ganio said.
To resolve the shortages, manufacturers will need to ramp up production to stock up pharmacy shelves, he said. He’s hopeful that at least some manufacturers will be able to quickly do that, thanks to new technologies.
Dr. Kerry Morrone at the Children’s Hospital at Montefiore in New York said she’s not heard from her patients or her hospital pharmacy of penicillin shortages yet. But she’s heard of shortages from her peers in other states, and that has alarmed her.
As things stand, the amoxicillin shortage is affecting sickle cell patients when they end up with a common complication called acute chest syndrome. The idea that penicillin, too, could possibly face a dire nationwide shortage terrifies her.
“We cannot let this happen. I’m dead serious,” Morrone said. “If there’s a short supply [of penicillin], I don’t know what I’m going to do.”
Sickle cell disease patients already face a litany of social and economic challenges everyday that makes it hard to get basic care. Being hit with a widespread penicillin would have huge ramifications, said Morrone.
“Children will die,” she said.
Invest in quality science journalism by making a donation to Science Friday.
Farah Yousry is a health equity reporter at Side Effects Public Media in Indianapolis, Indiana.
IRA FLATOW: This is Science Friday. I’m Ira Flatow. And now it’s time to check in on the state of science.
[MUSIC PLAYING]
SPEAKER 1: This is KPR–
SPEAKER 2: For WWNO–
SPEAKER 3: Saint Louis Public Radio.
SPEAKER 4: Iowa Public Radio news.
IRA FLATOW: Local science stories of national significance. Children with sickle cell disease rely on daily doses of penicillin to prevent infections. This is life-saving treatment. But it’s been hard to find penicillin lately in pharmacies. And while the FDA says there isn’t a shortage of the antibiotic, families and physicians are finding the opposite.
Joining me today to talk about this story is Farah Yousri, health equity reporter for Side Effects Public Media based at WFYI in Indianapolis, Indiana. Welcome back to Science Friday.
FARAH YOUSRY: Hi, Ira. Thanks for having me.
IRA FLATOW: You’re Welcome. Farah, just to review, remind us of what sickle cell disease is, if you will.
FARAH YOUSRY: Yeah. So sickle cell disease is a genetic disorder that mostly affects people of African descent. As many as 300,000 babies are born with it every year across the globe. That’s as many as babies born with HIV worldwide. But the awareness level surrounding both diseases is hugely different, as you can imagine. In the US, the CDC estimates that there are nearly 100,000 people with the disease, and most of them are Black.
So sickle cell disease is a blood disorder. People who have it find that their blood cells become misshapen. They turn from the typical doughnut shape that most of us have into the shape of a banana, or a sickle, hence the name, which means that these blood cells are not able to carry oxygen as well.
The blood cells also become stickier and harder to flow in vessels. And they can clump up and get jammed in some places in the body. And this could starve major organs of oxygen and could lead to strokes, organ failure, tissue damage.
And the hallmark of the disease is excruciating pain. And that’s typically known as pain crises. So these are episodes of extreme pain that patients need very high doses of narcotics for to be able to manage.
IRA FLATOW: Why do kids with sickle cell disease rely on antibiotics?
FARAH YOUSRY: So because sickle cell disease causes all these health problems and damage to the body, one way it also affects the body is it damages the function of the spleen. That’s the organ responsible for producing blood cells to fight germs in the body.
So babies in general have less mature immune systems and are vulnerable to illnesses. On top of that, if a baby has sickle cell disease, their immune system is severely compromised. So an infection that could cause mild illness in the general population can cause severe illness or even death for a little kid who has sickle cell disease. And it’s not hard to see how this plays out.
So as recently as the late 1970s, nearly one out of every three kids with sickle cell disease died before their fifth birthday. That’s a huge number. And all of this changed when a landmark clinical trial took place in the 1980s. The researchers put kids with sickle cell disease on prophylactic, or preventative, antibiotics, specifically penicillin. And they found stunning results. Kids were thriving. And since then, sickle cell disease moved from being considered a pediatric disease to a chronic illness, where people are living well into adulthood.
IRA FLATOW: Do we know why this antibiotic shortage is happening?
FARAH YOUSRY: So antibiotic shortages are actually more common than most of us realize in the US. But this current shortage of some of the most widely-used antibiotics like amoxicillin has been driven by a spike in demand. At least, that’s what experts who track these shortages and some drug makers are saying.
And it’s pretty unconventional compared to previous years, where there were shortages for other reasons. So this year, it doesn’t look like there are any manufacturing hiccups at the factories, for example. There aren’t any recalls of antibiotic shipments. At least, that’s not what’s driving the shortage. So it seems that there has been a surge in infectious diseases lately. Then, some manufacturers are reporting having some labor issues with drivers, shipping and delivery people who take the drugs to wholesalers and hospitals.
IRA FLATOW: What have you heard from people who have kids with sickle cell disease? I mean, how is this shortage impacting these families?
FARAH YOUSRY: Yeah. So kids with sickle cell disease typically rely on two daily doses of liquid penicillin. And that’s between two months until at least five years of age. Parents can put the penicillin doses in a medicine dispenser. It looks like a pacifier. The medicine is usually pink and sweet tasting for the kiddos to swallow.
So right now, as you said, the FDA did not say there’s an official shortage of penicillin in the US. But there are signs it’s getting harder. And supplies, especially of liquid penicillin, might be dwindling in some places.
I spoke with providers in many states and families who are finding it harder to get their hands on liquid penicillin. Dr. Seethal Jacob is a pediatric hematologist at Riley children’s hospital in Indianapolis. She says her patients have been hit by these shortages. And she worries that a widespread penicillin shortage could spell disaster for this vulnerable population.
SEETHAL JACOB: I’m worried that I’m going to be seeing more of our patients in the hospital with serious bacterial infections and obviously significantly concerned that some of them may become so ill that they would pass.
FARAH YOUSRY: And I spoke with one mother. Her name is Mary Warlo. She has a six-month-old baby boy called Calieb. He’s such a cutie. Smiling, laughing, chubby cheeks, curly hair. He has everything going on. And he takes his penicillin doses very peacefully. So the last time Mary went to fill her son’s penicillin prescription, she had to drive for hours all across Indianapolis. And she and her husband stopped by five different pharmacies until they were finally able to get their hands on it. Here’s what she had to say.
MARY WARLO: It’s just been really hard, I would say, trying to– there’s been a couple of days where he’s gone without it because we couldn’t find it. So then it’s a scare that if he doesn’t get it, if that affects him in other ways.
FARAH YOUSRY: She says she is terrified of what might happen the next time she goes to fill Calieb’s prescription. And that’s also been a concern for providers at big hospitals, who, some of them tell me their pharmacies are advising them to start looking for other alternatives.
IRA FLATOW: And so what are some of the solutions that people are turning to?
FARAH YOUSRY: So one thing some providers are trying to do is to prescribe penicillin tablets, which are very inconvenient because you have to divide them in half. And then parents have to crush them and put them in their baby’s formula or food and then hope the kid actually finishes the serving of food and not spit it or just throws it on the ground. And so already, some parents have started to do that.
Then the second best option for sickle cell disease patients, if they can’t take penicillin, is the antibiotic amoxicillin. I spoke with Dr. Monica Hulbert at St. Louis Children’s Hospital. And she says she tried to prescribe amoxicillin for some of her patients, and that was actually unsuccessful. They couldn’t find it, because amoxicillin has already been in short supply, according to the FDA. And so Hulbert tells me there are other less-preferable antibiotics patients can get on. But she worries about the ripple effects of this ongoing shortage. Here’s what she had to say.
MONICA HULBERT: The trick is that when one thing is unavailable, then everybody switches to the next thing. And then that also may– demand may exceed supply on that too.
FARAH YOUSRY: So for now, it’s uncertain penicillin. Shortages are not official yet. But several providers in different states across the country have told me their hospital pharmacies notified them that they are running low and advised them to start exploring those other options.
IRA FLATOW: Wow. Farah, thank you for taking time to present this story that sometimes flies under the radar.
FARAH YOUSRY: Thank you so much for your time.
IRA FLATOW: Farah Yousri, health equity reporter for Side Effects Public Media, based in Indianapolis, Indiana.
Copyright © 2023 Science Friday Initiative. All rights reserved. Science Friday transcripts are produced on a tight deadline by 3Play Media. Fidelity to the original aired/published audio or video file might vary, and text might be updated or amended in the future. For the authoritative record of Science Friday’s programming, please visit the original aired/published recording. For terms of use and more information, visit our policies pages at http://www.sciencefriday.com/about/policies/.
Kathleen Davis is a producer and fill-in host at Science Friday, which means she spends her weeks researching, writing, editing, and sometimes talking into a microphone. She’s always eager to talk about freshwater lakes and Coney Island diners.
Ira Flatow is the founder and host of Science Friday. His green thumb has revived many an office plant at death’s door.