Fact Check My Feed: What’s Up With These COVID-19 Mutations?
25:17 minutes
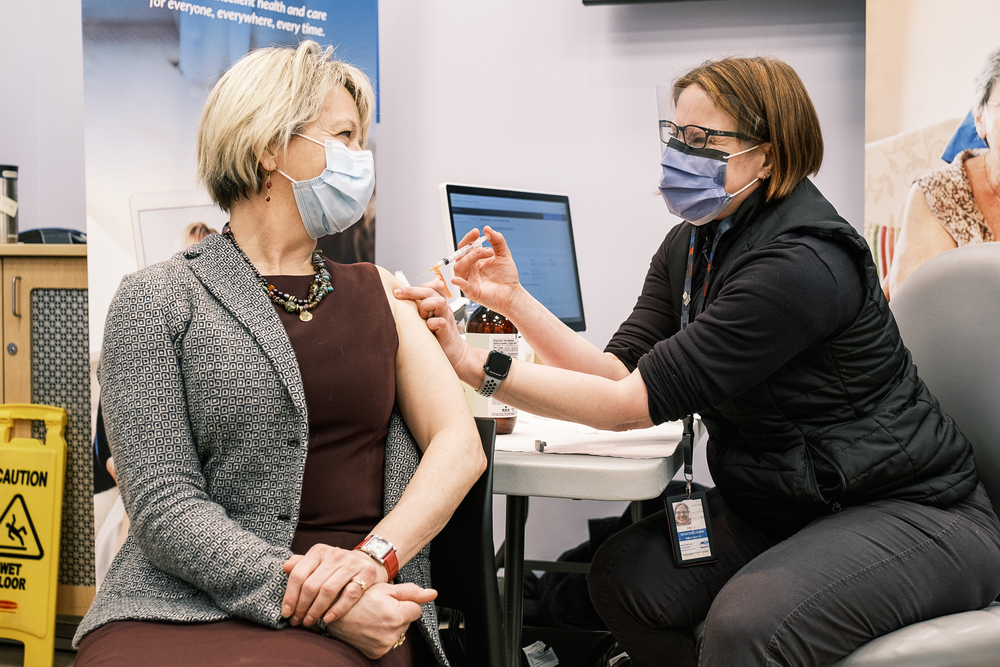
This story is part of Science Friday’s coverage on the novel coronavirus, the agent of the disease COVID-19. Listen to experts discuss the spread, outbreak response, and treatment.
It’s a new year, and that means there’s a whole slew of new COVID-19 news to dive into, including an overwhelming amount of new information about vaccines and mutations.
The U.S. has now administered roughly five million doses of COVID-19 vaccines, far behind the nation’s goal of vaccinating 20 million by the end of 2020. The two approved COVID-19 vaccines, one from Pfizer and one from Moderna, are intended to be given over the course of two doses. But there’s a discussion within the medical community about whether or not both doses are necessary for every patient.
Mutations are also an increasing concern. Variants from the U.K. and South Africa are concerning epidemiologists, and appear to be spreading. Though there’s no proof that either are more deadly, they may be more infectious.
Joining Ira to explain is Angela Rasmussen, a virologist at Georgetown University’s Center for Global Health Science and Security, based in Seattle, Washington.
Invest in quality science journalism by making a donation to Science Friday.
Angela Rasmussen is a research scientist at VIDO-InterVac, the University of Saskatchewan’s vaccine research institute in Saskatoon, Saskatchewan.
IRA FLATOW: This is Science Friday. I’m Ira Flatow. It’s a new week and a new year, and that means there’s a whole slew of COVID news to take a look at. All this new information about vaccines and mutations can be pretty overwhelming, right?
So we’re here to fact check your feed with our guest, Dr. Angela Rassmussen, a virologist at Georgetown University’s Center for Global Health and Security. She’s based in Seattle. Welcome back, Angela always great to have you.
ANGELA RASSMUSSEN: It’s always great to be here, Ira. Thanks for having me.
IRA FLATOW: You’re quite welcome. Let’s start with distribution of the vaccine for a minute. We’ve seen a lot of coverage that the US fell very short of its goal of vaccinating 20 million people by the end of 2020. In fact, we hear that just over 3 million doses were administered. Why did we fall so short?
ANGELA RASSMUSSEN: Well, I think one of the reasons we fell so short, and it is really complicated– I should add a disclaimer that I am not involved in any way in the distribution, so I only know about this from a bigger-picture level. But I think that one of the big problems that we’ve had with distribution is the fact that there really is no centralized vaccine distribution plan. Operation Warp Speed’s involvement in that really ends at the point where they allocate the vaccines to the different states. And at that point, it becomes each individual state or locality’s responsibility to distribute that vaccine, and some states are doing better than others.
For example, some states have implemented policies that actually make the vaccine much more difficult to access for some people. Such as New York, in which the vaccines are only to be given out at hospitals. Right now, when we have an unprecedented number of COVID patients going into hospitals, that makes using that environment to also distribute vaccines to healthy people very challenging. So it’s a really complex problem. It has a lot to do with logistics, and it also has a lot to do with all the different rules in the different places where the vaccines are actually being distributed on the ground.
IRA FLATOW: Yeah, we have no national policy that would be the same for everybody.
ANGELA RASSMUSSEN: That’s exactly right. And this was a problem that we also saw with testing. Each state– and sometimes local health departments– are predominantly involved in doing these tests and collecting the data, and then reporting it to a centralized federal data collator. And this has also really led to a lot of confusion, trying to look at the National numbers rather than the numbers by states. And so now we’re seeing the same thing with vaccine distribution.
It really does argue that for really important public health measures that affect all of us in the US, there really does need to be a federal national plan to unify us and to make sure that these things run smoothly.
IRA FLATOW: Do you think now that we’re getting a new president in a couple of weeks, things could speed up with the new administration?
ANGELA RASSMUSSEN: I really hope so. And certainly, President-elect Biden has made it clear that he does plan to have more of a federal plan. He plans to provide more federal leadership. And I really do think that’s what’s needed, because we shouldn’t be able to access really critical public health measures like vaccines based on the politics of who our local governor or leaders are.
IRA FLATOW: A few years ago when Tony Fauci was on the show talking about vaccinations– because we used to have him on regularly– he related a story that when he was a young child, I think he was six or seven, and he was living in New York. And there was an outbreak of smallpox in New York City. But because everybody used to get inoculated with smallpox– remember when you were a baby, they don’t do that anymore.
The infrastructure–
ANGELA RASSMUSSEN: –I am actually not that old, but I know the story.
IRA FLATOW: Well the infrastructure was there so that they could inoculate 8 million people in two weeks. I mean doesn’t that speak to us saying, hey, we’ve learned a lesson, we should create a permanent infrastructure because we’re going to have more outbreaks of viruses?
ANGELA RASSMUSSEN: Absolutely. And smallpox is a great example of that. That was the first vaccine. In fact, the vaccines are called vaccines because the virus that you use to inoculate somebody against smallpox, or variola virus, is vaccinia virus, or cowpox virus. So technically a vaccine is only really a smallpox inoculation because most vaccines are not based on vaccinia virus now.
Of course, we now use the term generally to mean an immunization. But I think that that’s a great reminder that we should maybe go back to basics. That sometimes, we need to be able to rapidly and dynamically and flexibly start vaccinating a lot of people, especially if there’s an outbreak of a re-emergent virus. Or if there is an outbreak of a new virus, now we have all these different vaccine technologies and we’ve shown, during this pandemic at least, that we can rapidly approve them for human use and that they’re actually quite efficacious. We need to start thinking about how we can do that as part of a larger, longer term pandemic and Epidemic Preparedness plan.
IRA FLATOW: We now have two approved vaccines here in the US– one from Pfizer, one from Moderna. These are both two-dose vaccines. And we have been hearing talk about whether or not both doses are necessary to try to stretch the vaccine supply out. What’s going on here?
ANGELA RASSMUSSEN: So that was first proposed before we started to realize what serious issues we were having with vaccine distribution. But the idea there was when those vaccines were submitted to the FDA for evaluation for emergency use authorization, both of them showed a certain level of protection after the first shots. And about 14 days after you get your first shot, there’s really measurable protection conferred by that one shot.
Now the caveat there is that we don’t know how long that protection would last after just one shot, because of course the clinical trials were evaluating them as two-shot regimens. So knowing that we would only have about 20 million doses of each by the end of 2020, people have proposed maybe we can give people one shot and that will confer some protection, and then either we could leave it at one shot or maybe we could give them a second shot just later on we have more vaccine supplies.
Now I think that there is merit to some of those arguments. But the real caveat there is that we don’t have any efficacy data on changing up the dosing regimen. So right now, given that we aren’t able to get the vaccines that we do have into people’s arms, I think it’s really premature to be suggesting that we just change the dosing schedules without doing any research to see if that would provide the same level of protection as the dosing schedules that were actually evaluated.
IRA FLATOW: And the UK, I understand, is trying this one-dose method right now.
ANGELA RASSMUSSEN: The UK is actually recommending a delayed second dose, so there is a difference with that. We do get many vaccines in what’s called a prime-boost regimen, where you get the first dose and then you get a booster shot later on. And for some vaccines, we know that you can get that booster shot over a large range of time. And in fact, one of the trials for the AstraZeneca vaccine did give the second dose up to 12 weeks later and didn’t see a measurable decrease in efficacy.
Of course, that vaccine is not yet approved in the US. However, the UK has also recommended that for the Pfizer vaccine, and there is no data about the effect that delaying a second dose might have. So again, this really falls into the category of something that we can think about, we can discuss. And if we do decide to move to this, we should actually test it before we start doing this at scale, because we really don’t know what the results would be from that.
IRA FLATOW: So we’re basically conducting a real-life experiment.
ANGELA RASSMUSSEN: That’s exactly right. And my other problem with this strategy is that I get that we are in a very dire, very urgent situation right now with the numbers of cases that we have. But at the same time, we aren’t really in a situation where the problem right now is vaccine supplies. So we don’t necessarily need to do that. Again, we need to work out the problems with distributing the vaccines that we already have before we try to figure out how we can protect more people by stretching the supplies that are limited.
IRA FLATOW: Aren’t there other one-dose vaccines in the pipeline? I’m thinking of like Johnson & Johnson.
ANGELA RASSMUSSEN: That’s right. So Johnson & Johnson is a different type of vaccine from the Pfizer and Moderna of vaccines. Those are mRNA vaccines that essentially give your cells instructions on how to make the spike protein from SARS-Coronavirus-2 that your immune system will then respond to. The Johnson & Johnson vaccine actually uses a different virus called an adenovirus that will replicate to a certain degree and produce that protein from SARS-Coronavirus-2. it’s thought that sometimes vaccines that involve actually some level of virus replication can induce alone, in one dose, those longer-term immune responses just because they are they’re more stimulatory to your immune system.
The Johnson & Johnson vaccine is in phase III trials that will probably read out this month, or at least in early February. And I believe that they’re evaluating both a two-dose and a single-shot regimen. So if that single-shot regimen shows efficacy levels anywhere near the Pfizer and Moderna vaccines, I think that might end this argument for good, because we’ll suddenly have a huge supply of an alternative vaccine that’s actually also easier to distribute than the mRNA vaccines because it doesn’t require the same sort of cold storage that those vaccines do.
IRA FLATOW: And J&J has the capacity to make a lot of vaccine, don’t they?
ANGELA RASSMUSSEN: They do. And the viral vector adenovirus system that they’re using– they’ve actually already developed as an experimental vaccine for HIV. So they already have the manufacturing capacity for that. They’ve further built that out as they were evaluating these vaccines. I think that could be a real game-changer, assuming that it does show the same level of efficacy that the Pfizer and Moderna vaccines did.
IRA FLATOW: There was some talk that when the Biden administration took over, it might sort of nationalize the vaccine production effort the way we did in World War II. We told the auto companies to make tanks instead of cars. Could you see that happening?
ANGELA RASSMUSSEN: I think so. I think that there’s been a lot of talk about using the Defense Production Act for both vaccines, as well as for components of the vaccine supply chain. So things like sterile saline, sterile liquids that are used to formulate the vaccines, glass vials and rubber stoppers, and syringes. All that kind of thing that people don’t think a lot about, but that are obviously really necessary for not only creating vaccines, but means to actually administer them to people. We’ve also heard a lot of discussion about using the Defense Production Act to make PPE for health care workers– and potentially also for the American people– to provide people with more means to protect themselves.
And I think all of those things would be a great use of the Defense Production Act. A lot of the time, I don’t like comparing public health measures to wartime measures, but in this case I think that we really should see a national effort to do those things. And I think that would be a great way of doing it.
IRA FLATOW: Help me understand something about the whole business about the coronavirus mutating. When we talk about it mutating, are we talking about an entirely different strain that we need to develop a new vaccine for, or what?
ANGELA RASSMUSSEN: So that’s a great question. And this is one thing I think that gets very confusing, that people often use the word “strain” quite a bit. But the word “strain” actually is not tremendously specific in terms of virologists. Some people will use it to mean a variant that’s genetically distinct, some people will use it to mean a variant that’s immunologically distinct, and some people sort of use it to describe different viruses that emerge in different places, for example.
If you looked at the different Ebola viruses that have caused outbreaks in the Democratic Republic of Congo, the 2018 Ebola virus would be a different strain from the 2016 Ebola virus that emerged there. So the term “strain” isn’t very precise and people use it, a lot of times, very differently. The variants that have been described so far in the United Kingdom and in South Africa– it’s debatable whether you want to call them a strain, but they’re genetically different. And they the key thing there is that they have a number of different point mutations and some deletions throughout the genome. What we don’t really know is what those different mutations do.
Now, it’s normal for RNA viruses like coronaviruses to acquire mutations every time they replicate. So it’s not surprising that we’re seeing a lot of different variants emerging, because the coronavirus unfortunately has had many opportunities to replicate since it spread so broadly through the population. What’s alarming about these two variants is that they seem to be more transmissible. Fortunately, they don’t seem to be more pathogenic. They don’t seem to make disease worse, but they do seem to be much easier to transmit to people, which is a problem for our health care system.
Right now we don’t know, actually, if they will have any effect on immunity produced by the vaccines, but they could. So far it’s looking more like the variant that was identified first in South Africa is more likely to have an impact on immunity. But those experiments are in progress and we don’t actually know that right now.
IRA FLATOW: I’m Ira Flatow. This is Science Friday from WNYC Studios. In case you’re just joining us, we’re talking with Dr. Angela Rassmussen, fact-checking your feed, all kinds of new information. It’s hard to keep track of it.
We saw Denmark kill millions of minks after discovering they had Covid. What other links to animals do we know of with Covid? Could it be dogs and cats? Or things that we just don’t know about or suspect?
ANGELA RASSMUSSEN: So that’s a very good question and one that I think about a lot, because it has long-term implications for controlling SARS-Coronavirus-2. So initially, this was probably not widespread throughout a number of different animal species. But we’ve since learned, both experimentally and in terms of animals being infected in the real world, that there are a number of different species that are susceptible to infection. So cats, minks, and ferrets– we know experimentally that hamsters are also susceptible. They’re used often as a model of pathogenesis, or the way that the virus causes disease.
Mice can be susceptible to some of these variants, including the variant discovered in the UK and in South Africa, and so on and so forth. So we know that there are a number of different animal species that can be infected with it. The real question long-term for me is, will the virus actually spill back into any of these species in the wild and start circulating there? That’s when things start becoming really unpredictable and you run the risk of having the virus be established in a new wildlife reservoir.
IRA FLATOW: Some flu viruses are carried by wild birds, are they not? Is there a possibility this could happen, too?
ANGELA RASSMUSSEN: Yeah so probably not with birds. To my knowledge, there aren’t any birds that have been discovered to be susceptible to SARS-Coronavirus-2. The natural host of influenza is migratory waterfowl and that’s one of the reasons why flu mutates so much, because it’s infecting these wild birds that are moving from place to place. And then it can also infect some livestock species, including domestic chickens and ducks, as well as pigs. And so that leads to a huge pool of different hosts across different species that can lead to the emergence of a bunch of different new influenza viruses and strains.
Fortunately, there’s not a bunch of different SARS-Coronavirus-2 circulating out there, at least that we know of. There’s no other subtypes of this virus as there is with influenza. But it is certainly a concern that some type of animal that does have a larger geographic range would be able to support this. And that could potentially introduce it then to other species, including humans. So this is all a big question mark right now, but it’s something we do need to think about over the long term. Because obviously, it has implications for controlling this virus if the virus is able to continue evolving in other species even after we mostly control-spread within the human population.
IRA FLATOW: So just to be sure, and to talk about it with our listeners, there’s no evidence so far that we should be worried about our house pets?
ANGELA RASSMUSSEN: No, not really. In fact, if anything, we should be worried about infecting our house pets, because cats can get somewhat sick. Dogs are susceptible to it but they don’t actually get very sick. And there’s certainly been no indication that there’s any dog-to-human transmission occurring, either. But so far, to my knowledge, there’s no reported zoonotic infections of SARS-Coronavirus-2 from domestic animals or house cats to people.
IRA FLATOW: We’re going to take a short break to digest a whole bunch of stuff that we heard. But when we come back, we’ll continue to fact-check your feed with virologist Dr. Angela Rassmussen. Stay with us. As I say, we’ll be right back after this short break.
This is Science Friday. I’m Ira Flatow. We’re back with Dr. Angela Rassmussen, virologist at Georgetown University’s Center for Global Health and Security. She’s based in Seattle, Washington. And we’re fact-checking your feed. We’re talking about the latest COVID news to start off this New Year, hoping to decipher all the stuff that we’ve been hearing.
Next question to you, Angela. About a quarter of the public is hesitant to take this vaccine, according to the Kaiser Family Foundation. And it’s not just anti-vaxxers. We’ve seen and heard stories of health care workers who are rejecting it, saying they don’t trust that vaccine to be safe and effective. What’s your take on this?
ANGELA RASSMUSSEN: Yeah, this is something I think about all the time, because the latest herd immunity threshold estimates that we need to achieve for vaccination is probably around at least 75% of the population. Which means we especially need those health care workers to take the vaccine if they’re able to. Now that said, I think it’s completely understandable that many people, including health care workers, are somewhat suspicious of the process. Because certainly, the federal government has not handled every aspect of this pandemic very well, and some parts not at all.
And people are aware that things like Operation Warp Speed implies that we’re going at this warp speed. That might mean we’re also cutting corners in terms of safety or efficacy. The good news to that is that while the process of reviewing the vaccines and approving them– or at least authorizing them for emergency use– was actually rigorous and not a lot was cut out of that compared to what we normally evaluate for other vaccines.
We were able to shave time off of this process by doing some things simultaneously rather than sequentially, as they normally would be done. There are some areas where we don’t have as much information, for example, about durability or how long the protection of the vaccines last. But what I keep telling people when I’m asked about this is that the Phase Three clinical trials, especially were the same size that they would be for any other clinical trial not done in this emergency scenario. There were tens of thousands of patients. They looked at safety very robustly.
They also showed surprisingly high efficacy. And by surprising, I mean that we didn’t really know how these were going to perform at scale. And they really exceeded our expectations. I think everybody was hoping for something around 70% would have been great, and these are 94% to 95% efficacious at preventing symptomatic COVID. So the phase III trials were actually great news, but they were also done in a way that allowed us to collect much of the data that we normally would collect, at least for in the short term.
So I try to educate people about that. But I think when you’re talking to people who are skeptical of the process or are hesitant about the vaccines, we need to really be thoughtful about the way we’re approaching people and engaging with them. We can’t write it off as, oh, you’re just not aware of the science or you’re skeptical anyways. We have to listen to people’s concerns and take them seriously, and address any questions that they have. And I think that it’s really important for people like myself as well as physicians and vaccinologists, immunologists, to really take these people seriously. To try to win hearts and minds rather than just wag our fingers and tell people that they should be taking it.
IRA FLATOW: Were you surprised, as I was, that something that normally we’ve been told takes about four years to develop? I mean, these two vaccines were developed and distributed within nine, 10 months.
ANGELA RASSMUSSEN: I’m surprised, just because so much has gone wrong with almost everything that we’ve tried to implement. But I’m very pleasantly surprised that this part of it did not go wrong. I think that, if anything, we can learn from this expedited approval process, It’s that maybe we should rethink the way that we’re evaluating some vaccines and drugs. Maybe it should actually take less time to evaluate some of these things. Maybe we should be doing preclinical studies, for example, in animals at the same time as we’re doing Phase I clinical trials for safety, because that did shave off quite a bit of time.
And ultimately, that shaves off a lot of costs as well. That makes it certainly easier for people to access these vaccines once they’re finally approved and thoroughly evaluated. And I think it also is a point worth making. I think most people don’t realize that once a vaccine is given full FDA approval, that doesn’t mean that we stop study.
People who get vaccines, including things like the measles, mumps, and rubella vaccine– which has been around for decades– they still study what happens when people get those vaccines. So we’re getting information all the time, even for vaccines that are already approved and have been on the market for years. So it’s not an abnormal process to keep studying these things after they’re being used in the general population. And maybe we should think about how we can balance the need for excellent scientific data before approval, but also the means get vaccines out quickly to a large number of people to improve public health.
IRA FLATOW: Have you received the vaccine?
ANGELA RASSMUSSEN: I have not. And in fact, I probably won’t until the summer or the spring– whenever it becomes available– since I’m relatively low risk. But I’m actually moving to Canada to take a job at a vaccine research institute there. And there I will be considered a front line worker so I’ll probably be able to get the vaccine as soon as I arrive in Canada.
IRA FLATOW: So I’m thinking about this. That you will then be a role model for people who say, look, there’s a health care worker– someone who’s actually a researcher– not fearful of taking the vaccine. Maybe you can convince those people that it is a safe vaccine.
ANGELA RASSMUSSEN: I think that’s really important. And many of my colleagues who are really health care workers now have been posting their vaccine selfies for that same reason. I think that’s especially important when you’re looking at people from communities of color. I think that in that case, there’s a lot of vaccine hesitancy– rightfully so– in those communities. Because not only is there a long history of medical and biomedical research exploitation of those communities, but currently, they’re being disproportionately affected by the Covid-19 pandemic because of racially-based health disparities.
So I think it’s particularly important for people of color, people from marginalized communities, to see people from within those communities also getting vaccinated, building that confidence. But I think overall, it is really important for people to model good public health behavior, including taking vaccines, letting people know, this is something I would do. I’m not asking you to do something that I wouldn’t do myself or that I wouldn’t recommend to my family. And I certainly am recommending to my entire family, including my parents and older people in my family, that they should get the vaccines as soon as they are able to do so.
IRA FLATOW: Well, Dr. Rasmussen, we have run out of time. We’d like to thank you, as always, for taking time to be with us.
ANGELA RASSMUSSEN: It’s always a pleasure to be here with you, Ira.
IRA FLATOW: Thank you. And please stay in touch as you move across the border to our neighbors to the North.
ANGELA RASSMUSSEN: I will, absolutely. That’ll be sometime in March or April. And I’m happy to come back via the airwaves any time.
IRA FLATOW: Dr. Angela Rassmussen, virologist at Georgetown University’s Center for Global Health and Security. She’s based in Seattle.
Copyright © 2021 Science Friday Initiative. All rights reserved. Science Friday transcripts are produced on a tight deadline by 3Play Media. Fidelity to the original aired/published audio or video file might vary, and text might be updated or amended in the future. For the authoritative record of Science Friday’s programming, please visit the original aired/published recording. For terms of use and more information, visit our policies pages at http://www.sciencefriday.com/about/policies/
Kathleen Davis is a producer and fill-in host at Science Friday, which means she spends her weeks researching, writing, editing, and sometimes talking into a microphone. She’s always eager to talk about freshwater lakes and Coney Island diners.
Ira Flatow is the founder and host of Science Friday. His green thumb has revived many an office plant at death’s door.