Fact Check My Feed: Why Are People Taking Discredited Horse Medicine For COVID-19?
12:05 minutes
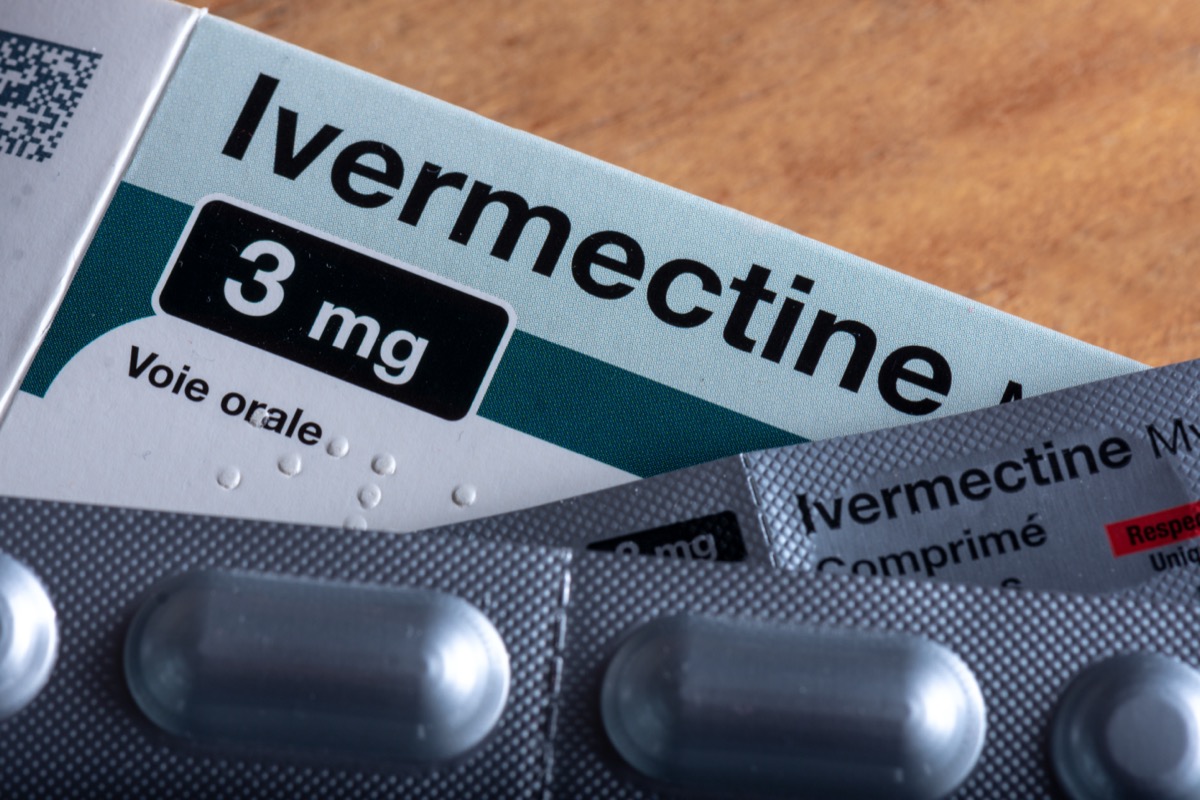
If you’ve been online at all in the past few weeks, you’ve probably seen discussion about the drug ivermectin. It was originally developed as an antiparasitic treatment for livestock, and in 2015, the Nobel Prize in Medicine went to scientists who found that it helped control parasitic diseases in humans as well. But recently, non-medical groups have been incorrectly promoting the drug as a treatment for COVID-19—even though the coronavirus is a virus, not a parasite.
Virologist Angela Rasmussen of the University of Saskatchewan joins Ira to look at the data behind sometimes hyperbolic COVID-19 claims, from the latest on booster shots to the emergence of a new coronavirus variant in South Africa.
Invest in quality science journalism by making a donation to Science Friday.
Angela Rasmussen is a research scientist at VIDO-InterVac, the University of Saskatchewan’s vaccine research institute in Saskatoon, Saskatchewan.
IRA FLATOW: This is Science Friday. I’m Ira Flatow. Later in the hour, a look at how global change is upsetting vital ocean currents in the Atlantic and a trip to the bakery for some sourdough bread geekery. But first, if you’ve been online at all in the past few weeks, you’ve probably seen discussions about the drug ivermectin. It was originally developed as an anti-parasitic treatment for livestock. And in 2015, the Nobel Prize went to scientists who found that it helped control parasitic diseases in humans as well.
But now some groups have been promoting the drug as a treatment for COVID-19, even though the coronavirus is a virus not a parasite. Joining me now to help unpack that and other news from your COVID news feed is Dr. Angela Rasmussen, Research Scientist at VIDO-InterVac, the University of Saskatchewan’s Vaccine Research Institute in Saskatoon, Saskatchewan up there in our friends in the north in Canada. Welcome back, Angela.
ANGELA RASMUSSEN: Thanks for having me back, Ira.
IRA FLATOW: OK. So what’s the deal with this horse medication story?
ANGELA RASMUSSEN: Ivermectin, in some ways, is really the new hydroxychloroquine. I’m not entirely sure how ivermectin came on the scene as a possible treatment for COVID-19. But multiple clinical trials have been conducted to look at ivermectin for treating COVID-19 or preventing COVID-19, and it doesn’t appear to do either one of those things. The FDA, as well as one of the manufacturers of ivermectin, Merck, have both released a statement saying that ivermectin cannot be used for treating COVID-19 and that people should not use it, especially as a substitute for vaccination.
And for me, like, months ago, when Merck said don’t take ivermectin for COVID, I mean, that’s not usually the kind of thing that a pharmaceutical company says about a product that they make, please don’t take our product. All of that along with the data is really a strong indication that ivermectin doesn’t do much in the way of treating COVID-19, and it certainly doesn’t prevent it. And it certainly is not a good alternative to vaccination. Now, some people who are promoting ivermectin for this purpose have said, well, ivermectin is on the WHO’s list of essential medicines. It’s a crucial medicine.
And you mentioned that the discoverers of ivermectin won the Nobel Prize because it is used for treating some really horrific parasitic diseases, one of those, onchocerciasis, African River Blindness, is a disease caused by worms that can ultimately result, as the name implies, in loss of vision. Most of the listeners probably are most familiar with ivermectin as an ingredient in Heartgard, or any of the other types of deworming medications that they give pets. It’s very effective for treating parasitic worm infections.
It is not effective, however, for treating COVID-19. And this is what really concerns me, are people who are promoting ivermectin as a valid alternative to vaccination for preventing COVID-19. And this is just simply not the case. If you’re taking ivermectin every day, not only if you are taking an off label can you suffer the consequences of taking too much ivermectin– because if you’re buying ivermectin in a dose that’s meant for horses or cows or large animals that have considerably more body mass than we do, you could overdose on it. But also you are going to continue to be vulnerable to COVID-19. And if you think that ivermectin is providing the same protection that a vaccine would, you’re going to potentially put yourself at a greater risk.
IRA FLATOW: Let’s move on to something that has a bit more evidence behind it, and that is boosters. There’s been a lot of talk about boosters, what Israel is doing, what other countries are doing. Will there be a third shot? Who will get it and when?
ANGELA RASMUSSEN: Yeah, this is really kind one of the hot topics of the hour. And really a lot of this is based on evidence that I was pretty skeptical of at first. But I’m starting to be more and more persuaded. We’re starting to see more evidence at really the population level that over time, the mRNA vaccines, and particularly the Pfizer vaccine, appears to be decreasing in effectiveness at preventing symptomatic COVID-19.
Now, this has been a really confusing topic, I think, because we are also hearing all the time about breakthrough infections and how they’re more common with the Delta variant. And that’s not necessarily due to this decrease in effectiveness. And that’s not always talking about cases as cases of symptomatic COVID-19. Sometimes it conflates symptomatic disease with PCR positivity.
But overall, this is really important. A decrease in effectiveness is something to be on the lookout for. Because in the clinical trials to evaluate these vaccines, they were expedited because this was an emergency situation. So we weren’t able to look at durability. We don’t know how long these vaccines are going to have a long-term protective effect.
And it is entirely possible that a third dose would always be needed because oftentimes one of the reasons why vaccine clinical trials take such a long time is they try multiple configurations of the dosing regimen to determine the optimal one for establishing durability. We have many vaccines that are three-dose regimens, usually with the third dose being given after a longer time interval from the second dose, which is really what’s being discussed now. The reason why this is important is not just to prevent asymptomatic breakthrough cases.
And I think this is one of the things that has really confused people because there has been some talk of, well, you’re moving the goalposts. First it was just to prevent COVID. And now it’s to prevent all these infections. And why do I care if I get infected if I’m just positive on a test and I don’t have symptomatic COVID?
But for people who are already high risk of developing severe COVID-19, an increase in the number of symptomatic COVID-19 cases in healthy low-risk vaccinated people probably means that there could be an increase in the number of severe COVID-19 cases in high-risk people who are more likely to end up in the hospital, more likely to die from having COVID. So it does make sense to say, well, we do have a surplus in many parts of the country of vaccines right now. We do have increasing evidence that a third vaccine, or even a mix-and-match vaccine regimen with a third dose is safe.
If you can increase vaccine effectiveness to take it from 50% to 70% back up to 90% in terms of preventing disease, that’s something that we would want to have. And then finally, as I mentioned before, many vaccine regimens are three-dose regimens. And the reason for that third dose– we are getting data to support this, too, for the COVID vaccines– is that if you have an increased interval between your second and third doses, your immune system basically says, you know what? This is something that I might continue to see, this pathogen. So I’m really going to exert the resources needed to really make that long-term memory protective immune responses.
And I hope that that’s what we will get from the third vaccine. Of course, we don’t for these vaccines because we weren’t able to look at durability. But knowing what we know from other vaccines and other types of vaccines, this usually applies, that sometimes booster doses are needed. But they’re not needed at frequent intervals, and they do result in immunity that lasts for years, in most cases.
IRA FLATOW: Can we learn anything from the Israeli experience on this? They’ve already been using third doses.
ANGELA RASMUSSEN: Well, absolutely. And unfortunately, what we can only learn is about the Pfizer vaccine in Israel because that’s predominantly the one that they’re using. But Israel has really been a wealth of information because they have had such a successful vaccine campaign, and they’ve been collecting so much data on it. So I think that probably we will be able to learn a lot more, at least about what the benefit is to a third dose from for the Pfizer vaccine at the population level.
IRA FLATOW: I hear you saying or implying that the Moderna vaccine may be longer lasting than the Pfizer vaccine.
ANGELA RASMUSSEN: Well, a study came out this week in The Journal of the American Medical Association that suggested just that. Now, there aren’t very many studies that are directly comparing these two vaccines. And I think people have assumed that they’re basically the same vaccine, as far as what the mRNA is encoding.
But there are a couple differences. The Pfizer vaccine is given in a lower dose, 30 micrograms compared to the 100-microgram dose of Moderna. And they have a different interval, three weeks for Pfizer, four weeks from Moderna. And they also use a different lipid nanoparticle to deliver the vaccine that ends up going into your cells where the spike protein gets made.
All three of those things could make a difference potentially. And that’s really what this study in JAMA showed. It showed that the Pfizer vaccine was reduced in terms of its effectiveness in people who’d received that compared to Moderna, and also that they had lower levels of neutralizing antibodies. So that may explain– so any of those things, the lipid nanoparticle, the interval, and the dose might explain why the Pfizer vaccine doesn’t seem to hold up for as long or be as durable as Moderna. But we still, of course, need to do more research.
IRA FLATOW: Let’s talk in the few moments we have left about news this week about a new variant called Mu and now in 48 states. Should we be concerned about that and other variants that we’re hearing about?
ANGELA RASMUSSEN: Yeah. So there’s been a lot of news about variants this week. And it’s been more along the lines of scariest kind of news, where oh, my god, there’s a new variant. It’s also got a Greek letter, which is now how the WHO has recommended naming the variants. It’s called Mu. And that’s just really because they’ve now gotten to M in the Greek alphabet.
There’s another cluster of variants called C.1.2 that’s a sub-lineage that was discovered in South Africa. This is a group of variants that has a lot of mutations that have accumulated in the spike protein. And there have been rumors going around that it mutates faster or that it’s the most mutagenic virus ever. None of those things are really true. And that’s not to say that these variants aren’t something we should be concerned about, something we should watch.
I think that’s why Mu is classified now as a variant of interest by the WHO. It’s not yet a variant of concern. And the reason why none of these are variants of concern yet is that we don’t actually know that we should be most concerned about them. What we are really going to have to see in the coming days and weeks is whether or not these variants start to outcompete Delta.
And that, to me, is really going to be the thing that we need to be most concerned about because we already know that Delta’s pretty bad. It’s more transmissible. It may be more virulent. It’s causing more breakthrough infections. It’s spreading like wildfire in places where people are unvaccinated.
If either of Mu or one of these viruses shows that it has the potential to do that even better than Delta, that’s what we really should be worried about. So we should be vigilant. But we shouldn’t freak out just because there’s a new variant on the block or a couple of new variants on the block. It really does remain to be seen whether they’re going to be a big bad or not.
IRA FLATOW: OK. Advice for not freaking out is a good place to end our discussion. We’ve run out of time. Thank you, Angela.
ANGELA RASMUSSEN: It’s always a pleasure, Ira. Thanks for having me.
IRA FLATOW: You’re quite welcome. Dr. Angela Rasmussen is a research scientist at VIDO-InterVac, the University of Saskatchewan’s Vaccine Research Institute in Saskatoon, Saskatchewan, Canada.
Copyright © 2021 Science Friday Initiative. All rights reserved. Science Friday transcripts are produced on a tight deadline by 3Play Media. Fidelity to the original aired/published audio or video file might vary, and text might be updated or amended in the future. For the authoritative record of Science Friday’s programming, please visit the original aired/published recording. For terms of use and more information, visit our policies pages at http://www.sciencefriday.com/about/policies/
As Science Friday’s director and senior producer, Charles Bergquist channels the chaos of a live production studio into something sounding like a radio program. Favorite topics include planetary sciences, chemistry, materials, and shiny things with blinking lights.
Ira Flatow is the founder and host of Science Friday. His green thumb has revived many an office plant at death’s door.