Probing Into The Microbiome In Your Nose
11:58 minutes
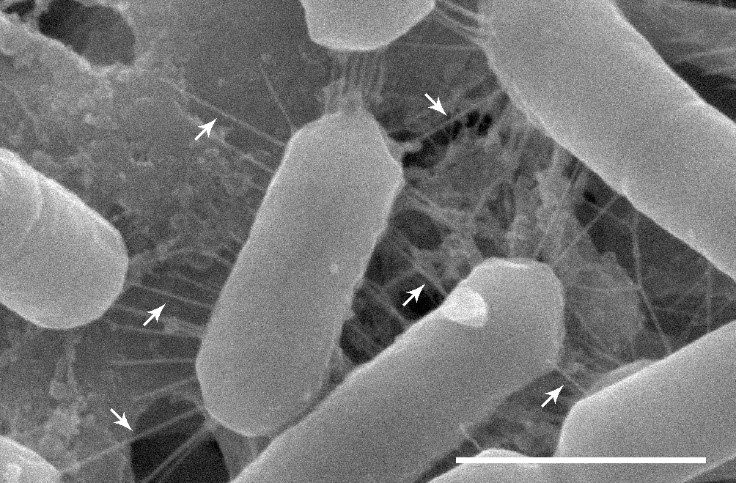
The human microbiome—our own personalized bacteria profile—plays a part in our health. The different parts of our body, from our skin to our gut, each have their own microbial profile. A team of researchers decided to explore the bacteria living inside our nose, publishing this week in the journal Cell Reports. Microbiologist Sarah Lebeer, one of the authors of the study, discusses what beneficial bacteria reside in our nose—and how this could be used to create a probiotic for upper respiratory infections.
Invest in quality science journalism by making a donation to Science Friday.
Sarah Lebeer is a professor of Bioscience Engineering at the University of Antwerp in Antwerp, Belgium.
IRA FLATOW: This is Science Friday. I’m Ira Flatow. Just a quick note before we get started. It’s been a while. We miss talking to you. I want you to say hello. So talk to us on the Science Friday VoxPop app on Twitter, or even email us scifri@sciencefriday.com.
And the Science Friday VoxPop app for this week, are you a health care worker feeling burnt out? We do want to hear from you. Maybe you’re dealing with a lot of COVID patients, or seeing layoffs in your workplace. Whatever is going on, if you’re a health care worker, tell us how you’re feeling. That’s on the Science Friday VoxPop app wherever you get your apps.
And now, what exactly lives inside of your nose? We’ve studied how the human microbiome, our own personalized bacteria profile, plays a part in our health, physical and mental. And we’ve heard a lot about the bacteria in our gut and in our skin. And now comes news of our nose. Researchers wanted to know what lives in our noses in the hopes of creating a probiotic for upper respiratory infections.
Their results were published this week in the Journal Cell Reports. And that is what my next guest is here to talk about. Sarah Lebeer is professor of bioscience engineering at the University of Antwerp in Belgium, author of that study. Thank you, Dr. Lebeer, for joining us.
SARAH LEBEER: You’re Welcome. Hello.
IRA FLATOW: Tell us briefly how you did this. You swabbed the noses and collected the nasal microbiome of over 300 people. What did you find in there?
SARAH LEBEER: So we had two groups. The first group was a group of healthy volunteers. And indeed, we swabbed their noses in what’s called the nasopharynx. I think the nasopharynx is now becoming very popular because– way popular because it’s also used for the COVID 19 swabbing. But it’s a place a little bit deeper inside your nose.
And then we had a second group where– it was for patients undergoing a surgery– a sinus surgery. Then they were swabbed during the surgery. The PhD student doing the research collected the samples.
IRA FLATOW: And what did you find? Did you find differences in people’s noses?
SARAH LEBEER: Yes, so that was– the plan was that we were going to look for differences between the healthy subjects and the diseased subjects. We had the most interesting findings were that the healthy subjects had more healthy bacteria in there, which are known as lactic acid bacteria.
IRA FLATOW: What is so important about the fact that they make the lactic acid?
SARAH LEBEER: Well, lactic acid is known as a natural preservative. It’s actually also what’s mating in yogurt and keeps your yogurt to have a longer shelf life, and milk, for example. So it’s able to kill the growth of unwanted bacteria. Seems to also have a communication capacity with host cells or our own human cells. Not everything is yet known on lactic acid.
IRA FLATOW: Is this the same kind of bacteria you would find in other parts of the body? The same stuff that’s growing in our noses?
SARAH LEBEER: You have related bacteria in other parts of your body, especially they’re quite dominant in healthy vaginas, healthy women. Normally, the vagina is dominated by lactobacillus species, they have a bit of a difference. But that’s also what we’re finding that in this article was that to adapt to the nose, the bacteria need to adapt or have some specific features. Because the nose is full of oxygen and has other special features.
IRA FLATOW: Since they’re at the part where– are there germs enter our noses, are they designed to fight off infections that might be entering our noses?
SARAH LEBEER: That’s one hypothesis we are– we have investigated in the paper. So they seem to have some evolutionary, maybe adaptation to help us fight pathogens. For example, they have this lactic acid, but they seem to also be able to produce other molecules that can help to reduce the growth of unwanted bacteria and even fungi.
And they also are able to communicate with certain receptors of our immune system. And they seem to have a more gate keeping or balancing rule for our use inflammatory reactions, for example, to other incoming particles or pathogens in the nose.
IRA FLATOW: It’s interesting that you mentioned that because they’re found in the nose that it might be interesting to study them because of a connection possibly to the COVID 19 infection.
SARAH LEBEER: Yes, that’s– it’s not only related to COVID 19, but of course, many viral infections but also many allergies. Allergies are also related to the incoming noxious particles our body has to react to. In fact, indeed, one of the following up questions we would like to explore is how your nasal microbiota impacts on your system’s ability to COVID 19, for example.
Based on my own research, I think it matters which bacteria live in your nose, and how you are able to fight the virus. A lot of research, of course, still has to be done to prove this hypothesis.
IRA FLATOW: It’s interesting because I was reading other research this week. There was a recent study looking in mice that found that mice fed lactobacillus had improved their memory. Are you familiar with that work?
SARAH LEBEER: Yes, I am. I’m familiar with that work and also previous work. Of course, if I read studies with mice, then especially memory, I think it’s very difficult to translate these findings to humans because humans are totally different and also their memory works different.
But it’s not so surprising that they can have an impact on memory. Because especially for the gut, it’s already known for decades that the bacteria in your gut can have an impact on your brain. And there is a gut brain axis. And indeed, another followups study of our work is that we would like to study the impact of your nasal microbiota on brain functions.
And let’s see whether we get funding for such studies. But this would also play a role.
IRA FLATOW: Now I know that you are, of course, one of the points of your work is looking to one day create a nasal probiotic. And you created a proof of concept probiotic in your study. Explain that to us, please.
SARAH LEBEER: Well, simple idea is maybe it’s possible to add beneficial bacteria to the nose of people with these chronic problems. But then, of course, you need to be able to culture this beneficial bacteria. You need to be able to formulate them in nose spray or a related device or related products. You need to make sure that it’s safe, and that the bacteria you apply in the nose can stick there and stay there. The nose is very efficient in clearing every particle that comes in.
We did a combination of screening the best bacteria that we thought that would stick to the nose, and also the bacteria would be dried and putting– and then later on put in a spray with saline, and then we test it. Of course, the safety with ENT specialists involved in the study.
IRA FLATOW: Now, I know there are a lot of strains of lactobacillus. Is it a specific strain that does its work, or does the general family of lactobacillus act in unison? Or do you really have to narrow it down to what strain we’re talking about?
SARAH LEBEER: That is a very good question. I think in this work, we find a specific strain with specific adaptations to the nose because we find it was, for example, [INAUDIBLE] positive. So it’s able to withstand oxidative stress levels. It also has specific genes that encode [INAUDIBLE] are special hair-like structure so that it can stick to the nose.
But the strain also has other properties such as lactic acid production and also [INAUDIBLE] molecules to interact with the receptors. And these more conserved properties are also present in other lactobacillus strains. So it could well be that other lactobacillus have similar function. So in the paper that’s coming out, we find another lactobacillus. It’s lactobacillus sakei, which have similar function, but it was not so good as the best strain we have. There are some conserved properties as really specific properties.
IRA FLATOW: How are we finding out how the microbiome– our microbiome communicates with the rest of the body? How does it do it? Does it do it in many ways, many different routes?
SARAH LEBEER: Yes, I think that’s a key message. So how bacteria interact with our human body is always through multiple mechanisms of action. So it’s not a single molecule interacting with one receptor in your body. Living entities with a lot of molecules, and it’s the sum of all these different interactions that plays a role. For example, in the case of this lactobacillus, they make this lactic acid, which is anti-microbial.
But they also cell wall molecules that interact with new receptors. Other molecules communicate with other virus-related receptors or other functions. So it’s very complicated to really [INAUDIBLE] and know how all these interactions are really happening or what’s happening. But it’s very interesting from a microbial point of view.
IRA FLATOW: Tell me about why it is so difficult. What are the obstacles in creating a probiotic?
SARAH LEBEER: First of all, you need to select a strain or a combination of bacteria that will be able to persist in the new body’s site. In this case, for example, for the nose, you want bacteria that will be able to stick to the nose wall for long enough time, but also don’t cause inflammation, don’t cause any problems.
Then, you need to make sure that they stay alive. I think that’s often one of the most difficult things. Probiotics are living creatures, living organisms. So you want them to stay alive. But also, it needs to be a product that is not perishable. That you don’t need to keep always in the fridge or in the freezer. So you need to make sure that in the product [INAUDIBLE] kind of sleepy state.
And then afterwards, they become reactivated, in this case, your nose. And then, you need to make sure that they have the desired function so that they’re active in your nose and that they have the right properties so that they reduce inflammation or they kill the bad bacteria or they promoted by a function of your nose or other body sites where you apply it.
IRA FLATOW: Do we have misconceptions about buying and consuming probiotics?
SARAH LEBEER: Oh, probably yes. I think there might be many misconceptions. I think often, especially for the gut, it’s also very difficult to really restore these biomes. And to really restore problems in your microbiome, I think that’s very difficult with a single probiotic. And also they don’t need to colonize to exert an effect. Based on my own research, I would say most– the main function of a probiotic is not to restore your microbiome, it’s more to have new multilateral effects and more subtle effects.
IRA FLATOW: That’s interesting. So it’s not that the probiotic works directly itself, but it helps to tweak up your immune system.
SARAH LEBEER: Yes. I think that’s a good summary.
IRA FLATOW: That’s interesting. That’s a great place to end, Dr. Lebeer. Thank you very much for taking time to be with us today.
SARAH LEBEER: You’re Welcome. Thank you.
IRA FLATOW: Sarah Lebeer is a professor of bioscience engineering at the University of Antwerp in Belgium.
Copyright © 2020 Science Friday Initiative. All rights reserved. Science Friday transcripts are produced on a tight deadline by 3Play Media. Fidelity to the original aired/published audio or video file might vary, and text might be updated or amended in the future. For the authoritative record of Science Friday’s programming, please visit the original aired/published recording. For terms of use and more information, visit our policies pages at http://www.sciencefriday.com/about/policies/
Alexa Lim was a senior producer for Science Friday. Her favorite stories involve space, sound, and strange animal discoveries.
Ira Flatow is the founder and host of Science Friday. His green thumb has revived many an office plant at death’s door.