Your Questions About COVID-19, Answered
You’ve had a lot of questions about the novel coronavirus. We’ve compiled answers and tips from health experts we’ve interviewed on the show.
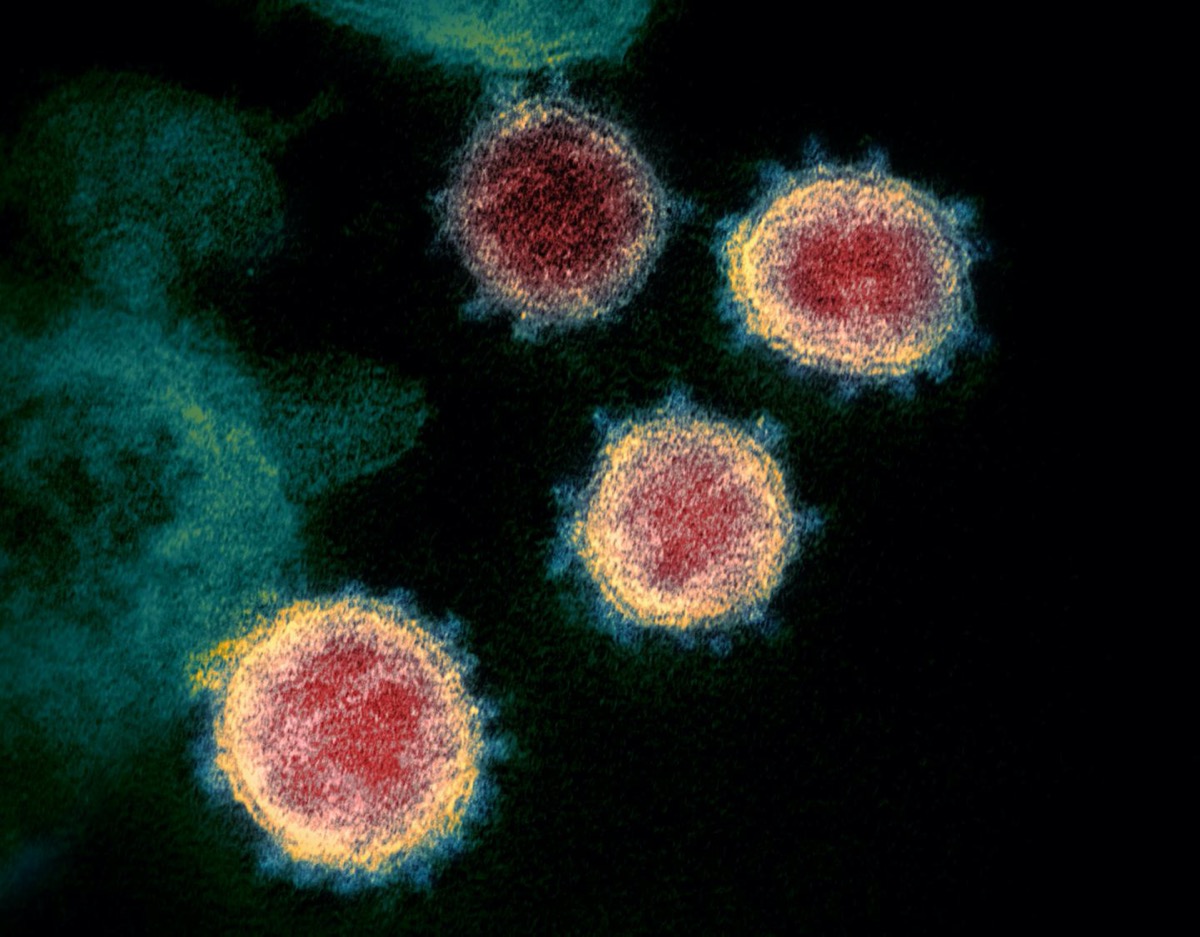
This story is part of Science Friday’s coverage on the novel coronavirus, the agent of the disease COVID-19. Listen to experts discuss the spread, outbreak response, and treatment.
This page will be updated with more answers from scientists as the story develops. Latest update: 7/8/20.
It’s been a hectic time, filled with lots of news (and rumors) about the novel coronavirus. Cases of its disease, COVID-19, have spread all over the globe. Nations are on lockdown and self-quarantine is slowly becoming the norm as daily life comes to a halt.
We’ve been covering COVID-19 since early January, when the outbreak began to grow in China. Since then, we’ve had many health experts and scientists on the show covering all aspects of the virus and its impact on human health—from tracking it and sequencing its genome, to advising appropriate public health practices.
To help guide you through all the information, we’ve compiled the most relevant questions Ira and our audience have asked. Before we dive in, follow the CDC’s prevention practices to slow the spread and lower your chances of getting the disease:
Research on COVID-19 and its virus has evolved rapidly in the span of months. As information changes, we’ll continue to add answers from scientists and public health experts we interview. Check back!
Basics
Transmission
Societal Impacts
Prevention
Treatment
Fact-Check My Feed
The Future
Answers have been edited and condensed for clarity.
How long does the virus live in an infected patient?
Scientists are still unsure. “As far as I’m aware, it has not been studied whether those patients are actually shedding infectious virus that could infect another person, [and] be transmitted to other people,” says Rasmussen. This means that any reports suggesting that the infectious living virus can be spread by a recovered patient for days or weeks are not supported by any current data.
Some of this uncertainty is due to what the coronavirus test looks for in positive cases. The most common test currently being used in the United States is a real-time reverse transcriptase polymerase chain reaction test, or RT-PCR test. A clinician inserts a long Q-tip up a patient’s nose to take a mucus sample at the back of the nasal cavity. That’s then processed in a lab to look for viral RNA.
“The test does not actually test for infectious virus. It tests for the virus’s genetic material,” says Rasmussen. “That means that those patients who have tested positive repeatedly after recovering from their symptoms have the virus’s genetic material in their cells. But that does not mean that they are producing infectious virus.”
To see how long someone may still be contagious, researchers need to administer more robust plaque assay tests. However, the process can take a couple days—not ideal for large-scale, rapid testing. It also requires a higher level of biocontainment and personal protective equipment that many clinical laboratories and hospitals are not equipped with, explains Rasmussen.
“The quantitative RT-PCR test that is used is much safer, and it’s much faster and it’s much easier to distribute to a wide variety of clinical laboratories.”
Do asymptomatic people go on to develop symptoms later?
“Some of them do. Some of them don’t,” Bushwick said. People who start out asymptomatic may go on to develop mild or severe symptoms. Or they might just stay asymptomatic, not even realizing that they were infected. “[Researchers] do know that there’s at least one outbreak that they traced to people who were infected but didn’t have any visible symptoms,” she says.
This information gives even more weight to the importance of social distancing, she adds. “The way to think about social distancing is not that you’re trying to avoid getting sick yourself, but assume that you have it and then you’re trying to keep other people safe,” Bushwick says.
Do recovered patients have immunity from COVID-19?
Virologists suspect that’s the case, but they aren’t completely sure. “We still don’t know that much about protective immunity to the virus,” says Rasmussen. In a study of experimentally-infected monkeys, the ones that were allowed to recover couldn’t be reinfected from the virus.
Human patients who’ve recovered from COVID-19 usually produce antibodies, which bind to the virus and render it inactive and non-infectious. Not every patient does have detectable antibodies, “but it really is a minority of the patients that have been studied so far that don’t have antibodies,” says Rasmussen. “So, the evidence thus far indicates that most people will develop an immune response. We assume that that’s protective, but we need to do more work to find out exactly how protective it is and how long that protection lasts.”
What should I do if I think I have symptoms?
“The best thing that you can do is that if you are sick, you should absolutely stay home and don’t go out and infect other people,” says Jennifer Nuzzo, a senior scholar and associate professor in the Center for Health Security at the Bloomberg School of Public Health of Johns Hopkins University.
If your symptoms worsen—if you become short of breath, for instance—she recommends contacting your healthcare provider to find the safest way to access care. “We don’t want people showing up unannounced. If they can get directed by their health care provider, that would be helpful,” she says.
How easily does the virus transmit?
“It seems pretty transmissible,” says Helen Branswell, a senior writer covering infectious diseases at STAT. For every one person affected, they could infect two to five people, “which is a pretty brisk level of transmission,” Branswell says. “This virus is very efficient at spreading from person to person.”
“The best thing that you can do is that if you are sick, you should absolutely stay home and don’t go out and infect other people.” — Jennifer Nuzzo
Is it true that older people only get really sick from the virus?
Initially, the messaging from health authorities was that the virus was more likely to affect older people. But the governor of California said that half of their cases are in people younger than 50. “I mean, look at nationwide cases,” says Maggie Koerth, a senior science reporter at FiveThirtyEight. “You’re still talking about a very lopsided hockey stick pattern, where the older you are, the more likely you are to have symptoms, to have been hospitalized, to have died,” she says. “But there are a lot of younger people who seem to be getting this too.”
Are infected people who don’t have symptoms spreading it more than those who are visibly sick?
It seems to be that way. Sophie Bushwick, technology editor at Scientific American, said that at the beginning of the month, health officials believed most of the virus spread came from people who were showing physical symptoms. “But more and more studies have been coming out that suggest people with no symptoms at all could be spreading the virus,” she says. “In fact, some people who were infected with the virus and not yet showing symptoms [asymptomatic people] had what’s called ‘a higher viral load.’ That means there’s more that they produce.”
For instance, if an asymptomatic person were to cough, a droplet of saliva from that cough would have more virus in it than from someone who was showing symptoms.
How are Black, Latino, and Native American people at higher risk of infection?
There are many different factors—many of which reflect pervasive disparities, says Uché Blackstock, physician and founder of Advancing Health Equity in Brooklyn, New York. Black, Native American, and Latino people have disproportionate rates of COVID-19 infection and death. Access to quality health care, paid sick leave, adequate housing, and occupation all contribute to health and risk of exposure.
“One thing that I did notice, not only were we seeing more Black and Brown patients starting in mid-March, but less white and affluent patients—and many of those patients had the luxury of working remotely from home,” Blackstock says.
“The structural racism has essentially made these communities sick. So when you have a pandemic and a crisis like this, it’s essentially a crisis within a crisis.” — Uché Blackstock
Many patients are also essential workers, putting them at even higher risk of contracting the virus. Construction workers, farmers, truck drivers, transit workers, grocery clerks, and many service workers who still have to report to work are largely people of color, says David Hayes-Bautista, director of the Center for the Study of Latino Health and Culture at UCLA’s medical school. Native American communities have also been hit hard by the outbreak, yet data is not being collected consistently to evaluate the impact, and the Indian Health Services continues to be underfunded, says Rebecca Nagle, journalist and citizen of the Cherokee Nation in Tahlequah, Oklahoma.
“It’s funded at about 16% of what tribal leaders and Native health experts say it’s needed. And so that’s created this gulf of health disparities that leaves Native Americans more vulnerable to coronavirus.”
These trends are not new. It’s a continuation of the historic racial inequities in health care, Nagle, Hayes-Bautista, and Blackstock say.
“When you look at the underlying health conditions that the CDC lists, things like asthma and diabetes, Native Americans rate the highest. And that comes from years of racial inequity in access to health care,” says Nagle.
“Up until the second week of March, ICE, Immigration Customs Enforcement, was going into hospitals here in Southern California and extracting folks to deport, which then tends to depress someone’s willingness to go into a medical facility for whatever reason,” Hayes-Bautista says. “We have all these structural things and then wonder why are Latino and African Americans having higher rates. Well, it’s not that we’re weaker. It’s just that this shows the structure of the system. We’re more exposed. We have less access to care.”
“The structural racism has essentially made these communities sick,” Blackstock adds. “So when you have a pandemic and a crisis like this, it’s essentially a crisis within a crisis. And so it’s these most vulnerable communities that end up suffering the most, which is why we’re seeing these incredibly high mortality rates in Black and Latino communities.”
How can the government address the decades of structural racism in health care that COVID-19 is exacerbating?

“We have to have a decades-long commitment,” says Anthony Fauci, director of the National Institute of Allergy and Infectious Diseases and a physician who has consulted the government on COVID-19, Ebola, AIDS, and past outbreaks. Communities burdened with improper healthcare provider practices, housing, working conditions and other social and environmental determinants have increased risk of chronic health issues.
“Those are the kinds of things that we need a long-term commitment to, because they’re not going to go away spontaneously,” Fauci says. Community outreach and education on public health, such as vaccination and treatments, is also essential in connecting with populations who have been historically mistreated.
“We have a very special effort to do outreach to minority communities, not only African Americans, but Latinx, and Native Americans, because those are the minority populations that always seem to get the short end of the stick on things,” he says. “We want to make sure they understand that this is something that could be very beneficial to them, particularly since as we know that with coronavirus, there’s a disproportionate burden of infection and complications leading to serious outcomes among the minority populations, particularly African Americans.”
“One of the things that might be a positive is that this has shed a very bright light on the disparities that we’ve known about for so long, and how destructive and harmful these disparities are to the African American population. So, I would hope that this would re-energize us in a commitment to do something about that.”

Why is soap the best way to protect against the virus?
“Soap is important,” says Benhur Lee, a professor of microbiology in the Icahn School of Medicine of Mt. Sinai Hospital in New York City. “Its molecule has a polar end, meaning it likes water, and a nonpolar end, a hydrophobic end that does not like water.”
Those hydrophobic and hydrophilic ends disrupt the molecular bonds in grime and the coronavirus cell, which we can collect on our hands as we touch things throughout the day. The coronavirus has a lipid membrane, Lee says—basically a layer of fat protecting the virus from the outside world.
The hydrophilic, polar “head” of soap loves to bind with water molecules due to their opposite charges, while the hydrophobic tail doesn’t have a charge. The tail latches with the fatty, lipid membrane that envelops a coronavirus cell, breaking it down.
“The cell membrane is a kind of a fat itself, and so soap dissolves the fat. And with water, it washes it away,” Lee says. So the soap binds to the molecules and drags all of them down the drain when you rinse.
28/39 Soapy water is totally different. Soap contains fat-like substances knowns as amphiphiles, some structurally very similar to the lipids in the virus membrane. The soap molecules “compete” with the lipids in the virus membrane. pic.twitter.com/roMbcOnDr2
— Palli Thordarson (@PalliThordarson) March 8, 2020
What should I be using more, soap or hand sanitizer?
“Hand sanitizer is going to reduce the number of microbes on your hand, but it’s not going to eliminate all of them,” says Popescu. While she recommends hand sanitizer as one way to neutralize the virus, hand washing still wins out. “You really need to wash your hands every few times that you use hand sanitizer, because that mechanical motion of soap and water for 20 to 30 seconds, that’s what’s going to get rid of a lot of that bioburden that microbes like to grow on.”
Should I be making hand sanitizer if I can’t find it?
“I am personally not a big fan of that,” says Popescu, “simply because there’s a lot of room for error, and most of us aren’t great chemists when mixing our own things.” She says when you’re looking for it in the store, look for sanitizer that has at least 60% ethanol. “If you are not getting that minimum of 60%, it’s not going to be [efficient]. And that can be very misleading, and give you a false sense of security.”
“That mechanical motion of soap and water for 20 to 30 seconds, that’s what’s going to get rid of a lot of that bioburden that microbes like to grow on.” — Saskia Popescu
How long can the virus live on surfaces?
“Anywhere from an hour to days, depending on the type of surface. A recent study conducted by the National Institutes of Health found that COVID-19 is stable “up to three hours as aerosols, up to four hours on copper, up to 24 hours on cardboard, and up to two to three days on plastic and stainless steel.”
These experiments were conducted in relatively high humidity (40% on surfaces, 65% for aerosols). The virus appears to survive longer in lower humidity. “In our households, the humidity of the air is quite low, around 20% relative humidity,” says Akiko Iwasaki, a professor of immunobiology at the Yale Medical School. “So it’s expected that these viral particles that are in the air can survive for even a longer time period than an hour.”
As Angela Rasmussen, an associate research scientist in the Columbia University Mailman School of Public Health, pointed out though, you shouldn’t take those numbers to the bank. “They’re completely dependent on the conditions that those experiments were done in. What we don’t know right now is how other temperature or humidity conditions would affect those things.”
Should I be cleaning the surfaces in my home?
Yes. “Surface cleaning and disinfection is really important during this time because it’s still flu season,” Popescu says. “And if you touch a dirty surface and you don’t clean your hands and then you touch your eyes, that’s a great way for organisms to transmit.”
What kind of disinfecting wipes should I look for?
Look for wipes that say that they’re EPA registered disinfectant, Popescu says. That registration means that it works on emerging viral pathogens, like the novel coronavirus.
Can I use disinfectant wipes on my hands?
No. “It is so important that people don’t use disinfectant wipes on your hands as a cleaning tool,” says Popescu. Those wipes are filled with harsh chemicals—and it’ll hurt your hand. “It would be like if you used a ton of hand sanitizer in a couple of minutes.” That causes your skin to dry out and your skin cells to breakdown—putting you more at risk. Popescu recommends that you rinse your hands after you use a wipe. “Clean surfaces with them, but don’t use it as a wipe just on your hand,” she says.
How can I disinfect my clothes?
Keep doing your laundry. Regular laundering—washer and dryer—is a normal disinfectant procedure at hospitals. The important step is the dryer. “Your normal dryer should be fine,” says Popescu. “100 to 130 degree Fahrenheit for 30 minutes in a dryer tends to kill most microorganisms on clothing.”
Line-drying doesn’t work as well—even with the microbe-killing UV light the sun puts out. “I would say that would work maybe during an Arizona summer,” she says. But the high temperature that a dryer provides is a key help.
If I have to fly or travel, what are the best ways to stay safe?
The White House recommends against gatherings of more than 10 people —a Boeing 737 holds more than 17 times that number. But if you absolutely have to fly, try to book a window seat. “You’re most at risk from the people that are seated one row ahead of you, one row behind you, and two seats on either side of you,” says Vicki Stover Hertzberg, a professor and the director of the Center for Data Science in the Nell Hodgson Woodruff School of Nursing at Emory University. “By booking that window seat, you eliminate all those people to one side of you at least.”
She also cleans her seat and tray table with a disinfectant wipe, doesn’t move from her seat while flying (to reduce exposure to people in the plane), regularly uses hand sanitizer to keep her hands clean, doesn’t touch her face, and stays well hydrated. And she doesn’t turn on the vent above the seat.
In an ordinary environment, if someone coughs or sneezes, the spittle goes about three feet in front of them and gravity does the rest, taking it to the floor. “But if you’ve got that vent from above coming down at you, it’s going to attract those droplets from the person next door to you or another seat away and bring them into that airstream and then [you’d] be putting them all over your face,” Hertzberg says.
How does contact tracing help slow the spread of disease?
“Contact tracing is intended to break chains of transmission among people,” says Crystal Watson, a senior scholar in the Center for Health Security and an assistant professor of Environmental Health and Engineering at Johns Hopkins University. This is how contact tracing would work: When someone becomes sick, they are quickly isolated (either in their home or hospital, depending on the level of medical care they need). Then, a public health worker asks them who they’ve had contact with during the time they may have been infectious, and the worker reaches out to those contacts.
Those contacts are asked to stay home and quarantine for two weeks. If they can’t do that, they offer them another facility to quarantine safely. “But the idea is that they are then staying out of circulation in the community,” Watson says. “And if they are indeed infected, then hopefully they won’t be passing along that infection to other people.”
Can I donate homemade masks to hospitals?
It depends on the hospital, but most seem willing to take them. “We always want to have a backup,” said Rob Poirier, the clinical chief of emergency medicine at Barnes Jewish Hospital and the Washington University School of Medicine in St. Louis. Healthcare workers always use the CDC-approved PPE first. Cloth masks are advised to use only as a last resort. Still, his hospital is accepting donations for homemade PPE—just in case. “If, for some reason, we run out of all the hospital supplies, we would definitely use the homemade supplies if it came to that.” Check with your local hospital first before trying to donate homemade masks or other medical supplies.
Why does it take so long to develop a vaccine?
The main concern is making sure it’s safe. Currently, vaccines are first tested on animals. But “right now, there’s not even an established animal model for this disease yet,” says Branswell. Next, “you have to test it in people to see if it’s safe, and then you have to test it in more people to see if it works.” After a vaccine clears safety and effectiveness, a mass production cycle needs to be put in place.
“It’s not like you can commandeer company X’s vaccine production line to make a vaccine. You have to figure out where it’s going to be produced. And all of that takes time.”
On February 18th, Sanofi, a major vaccine manufacturer in France, said they were going to try to make a coronavirus vaccine. The developers estimated that the fastest they could have a vaccine available is in three to four years, Branswell says. “I think that’s probably a more realistic timeline than people like to hear.”
Should I not take ibuprofen if I’m sick with COVID-19?
There is currently no evidence that suggests that ibuprofen worsens the conditions of COVID-19.
“Even the World Health Organization—which several media outlets had cited as saying you should avoid ibuprofen—is now saying they never said that and they’re, in fact, considering ibuprofen to be safe for COVID patients,” says Koerth.
The speculated association all started with the French health minister stating in mid-March that four young people with the virus developed more severe symptoms after taking the medication. And there had been at least two large trials in the past that suggested that ibuprofen can exacerbate general respiratory illnesses, as noted by the British Medical Journal.
“But right now, other researchers are saying there’s not really any evidence that SARS-CoV-2 is doing that with ibuprofen,” Koerth says.
Learn more about which proposed COVID-19 treatments are backed up by science on our most recent #FactCheckMyFeed segment, including remdesivir, hydroxychloroquine, blood infusions, vitamin C, and HIV treatment.
What are the incorrect claims in the viral “Plandemic” video?
“Almost everything,” says Rasmussen. During the week of May 15, a video made the rounds on YouTube, Facebook, and other social media channels that had brow-raising claims about the pandemic. It was taken down shortly after public health experts and researchers pointed out its baseless and false information. Rasmussen emphasizes that the claims that the pandemic had been planned and that vaccines are ineffective are false.
“It’s very dangerous, I think, to circulate the idea that vaccines or any hypothetical vaccine that will be developed against SARS-CoV-2 is all part of this dangerous conspiracy to kill people because then people might not get the vaccine, and getting that vaccine will be key to us resuming our normal lives,” Rasmussen says. “We’ve already seen with measles vaccine denial, for example, that one consequence of this is actually people can be very seriously ill. And people can die.”
Do scientists know that the virus is natural versus from a laboratory?
There is substantial evidence that the virus was not made in a lab, Rasmussen says. It also did not “escape” from a lab and was not created as a biological weapon, as some like to theorize, she adds. “The evidence, just by looking at and analyzing the genome strongly, strongly suggests that this virus emerged naturally,” she says. While researchers are still tracing exactly where the virus came from and how it was transmitted to humans, there is strong evidence that it originated from bats, Rasmussen said.
“We know that people who live near bat caves in China, a number of them have antibodies to other bat SARS-like coronaviruses,” she says. “Serology data suggest that this happens with a fair amount of frequency. So it’s entirely possible that any number of natural encounters with either a bat or their droppings or another animal, potentially, that was infected with SARS-CoV-2 was actually the event that led to this, rather than an escape from a lab.”
Is it possible to establish herd immunity?
Historically, herd immunity has been created with vaccination, says Rasmussen. Herd immunity happens when there are enough people in a population that become immune—not susceptible—to a virus, which prevents it from spreading.
“The main reason that vaccines have been such incredibly powerful public health tools is that they allow us to get that immunity without having to suffer the deaths that will happen if we were actually infected with those viruses themselves,” says Rasmussen. “I think it’s really, really dangerous to talk about herd immunity as let’s just reopen up and infect everybody.”
How do I know what to believe on social media or what scientific papers to trust?
Be wary—misinformation is rife on social media. The Center for Disease Control and the World Health Organization are the most reliable sources, Rasmussen says. But if you’re looking for more information in articles, there are ways you can detect fake news. She recommends that you search who’s being interviewed, what their experience is, and what scientific papers they’ve written. “If you Google me,” Rasmussen says, “you can find out that I’ve worked on MERS, Coronavirus, and Ebola, and so forth. You can see that I have an appointment at Columbia University. Therefore, I might be a more trusted source to ask about virology than somebody who has a different area of subject matter expertise.”
But another wrinkle in spotting good information from the bad lies in a scientific paper publishing method that wasn’t around during the ebola outbreak a few years ago: preprint servers. “Preprint servers are a great way for scientists to get their manuscripts and their data out to the public prior to undergoing peer review, which can be a lengthy process,” Rasmussen said.
This helps with getting important information out faster, but the problem is the increasing volume of papers being posted on these servers. There are so many that it’s “very difficult to know which of those papers are good quality science, and which of them needs some more work or are just generally bad. And there have been several examples of that.”
One of those examples was a study (which ended up being published in the Journal of Medical Virology) that suggested that this coronavirus emerged from snakes. However, it was based on a flawed analysis, Rasmussen said. “But because it was posted on a preprint server, it had the appearance of a legitimate scientific manuscript. And that is one of the troubles of people who are not as experienced with reporting on scientific issues: being able to distinguish papers such as that one from other really excellent papers that have come out on preprint servers.”
Will the new coronavirus go away as the temperature warms?
Currently, it is too early and difficult to predict if the emerging virus will follow a seasonal pattern like we see with illnesses caused by other kinds of coronaviruses, such as the virus of the common cold, says Iwasaki.
However, past research by Iwasaki and her team has found that other viruses, like the influenza virus, don’t survive as well in humid conditions. Raising the humidity of indoor environments by about 40% to 60% could help clear the viruses from the respiratory tract better, she suggests. “I think there is an intervention that we can do, which is to humidify homes or offices or hospitals in order to reduce the impact of the disease within the human population.”
If this is a seasonal virus, could it come back next year?
“Yes, it’s entirely possible,” says Iwasaki. “We’ll have to see what happens next year. But it’s possible.”
Invest in quality science journalism by making a donation to Science Friday.
Dee Peterschmidt is Science Friday’s audio production manager, hosted the podcast Universe of Art, and composes music for Science Friday’s podcasts. Their D&D character is a clumsy bard named Chip Chap Chopman.
Lauren J. Young was Science Friday’s digital producer. When she’s not shelving books as a library assistant, she’s adding to her impressive Pez dispenser collection.